A fragmented approach to child health is damaging the long-term health of the UK, warns President of The Royal College of Paediatrics and Child Health, Professor Russell Viner
The pressures on the health service are well documented – increasing demand and a workforce that’s not expanding at the same pace. Alongside this, there have been significant cuts to public health budgets which mean preventative child health measures are not being prioritised. This presents a hugely worrying picture; a health service focused on dealing with acute need and a lack of resources being put into preventing ill health. It’s a viscous cycle that needs to be broken, otherwise current and future generations will face increasingly ill health and the financial burden on the NHS will continue to grow.
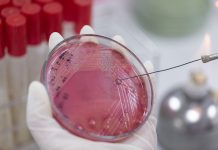
Preventing ill health means getting health right during childhood. We know that the UK has some of the poorest child and adolescent health outcomes in Europe – in areas including mortality, diabetes hospital admissions and obesity rates. The RCPCH’s State of Child Health report, published in January 2017, set out in stark terms the fact the UK is failing its children and young people when it comes to their health – despite having one of the best health systems in the world, and some of the best trained doctors and other health professionals.
At the beginning of this year, The Royal College of Paediatrics and Child Health (RCPCH) launched its ‘State of Child Health: One year on’ scorecards for England, Scotland and Wales which describe progress made against the recommendations made in its landmark ‘State of Child Health’ report.
The scorecards for Wales and Scotland show their respective governments are making great strides in enacting policies to improve child health – and much more so than central government. Wales is making good progress on protecting children and young people from the dangers of tobacco, extending bans in public places to school ground, NHS sites and playgrounds and has made some exciting developments linked to child health research. It is also reforming the curriculum to provide real opportunity to improve health and wellbeing and sex and healthy relationship education – as young people consistently say they need – and is developing a strategy to help tackle obesity.
In Scotland, there has been commitments made in relation to child poverty – the passing of the Child Poverty (Scotland) Act with defined poverty reduction targets, on mental health – a strategy is in development – and there has been a commitment from Scottish Government to ensure specialist breastfeeding advice and support is delivered to women. The Scottish Government has also made commitments to expand the number of health visitors and to review statutory sex and relationships education in all schools.
For England, the very useful Childhood Obesity Plan, brave legislative action in the form of the soft drinks industry levy, the launch of a Digital Child Health Strategy, the publication of a new Tobacco Control Plan and the initiation of some specialist paediatric service child health. However, Westminster is still not giving children and young people’s health the political attention it deserves in comparison to the Scottish and Welsh Governments.
In England, the scorecard revealed there had been no improvement in several fundamental areas including:
- No plans for an overarching child health strategy;
- No junk food advertising ban;
- No way of measuring UK breastfeeding prevalence and;
- No increased investment in child health research.
Of major concern are the deepening public health cuts which have worsened in the last year and are disproportionately affecting children’s services. The scorecard marks this ‘black’, quoting latest statistics that show public health spending is over 5% lower in 2017/18 compared with 2013/14.
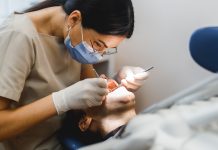
Take health visiting services for example. These services are vitally important for early identification and prevention of health and wellbeing issues and they are at risk of being lost entirely. Health visitors provide new mothers with breastfeeding support, health and nutrition advice and developmental advice for their baby. They also act as a tool for identifying parents who may be at risk of developing mental health problems. We need central government to give these services the attention they deserve by investing heavily in them, preventing ill health rather than trying to fix it later in life, which is often at a much greater expense.
Getting to grips with this country’s obesity crisis is another example of where investment in prevention provides greater savings later in life.
Four-fifths of obese children will remain obese as adults and this will result in them losing between 10-20 years of healthy life. What’s more, these adults are also more likely to have overweight or obese children. The cost of treating obesity is astronomical – in excess of £6 billion. For the sake of the nation’s well-being and the financial stability of the health service, the government must get to grips with these kinds of challenges and move its focus from the short-term and ineffective to long-term and productive.
There are many factors that lead to obesity, but one that has a significant affect is the marketing of unhealthy foods. We know that young people are hugely influenced by the adverts they see on television. They are much more likely to purchase these products or pressure their families to make the purchase and the food industry knows this. The top 18 spending crisp, confectionary and sugary drinks brands spent over £143 million advertising their products in 2016. The government must crack down on this by restricting the advertising of foods high in sugar, salt and fat before 9pm and protect those most vulnerable.
Investing in children is an investment in the entire population. A year has already passed since the RCPCH launched its flagship report on children’s health. Meanwhile, the state of child health continues to stumble, and services continue to struggle under the pressure. The government must put children and young people first- and not fall victim to political short-termism. A ‘child health in all policies’ approach would ensure that the health implications for children are considered in whatever policy is implemented, resulting in a longer-term benefit for the population as a whole. We also need equality of priority for children’s health with adult health. It is time for real parity between child and adult health because prevention is often much safer, cheaper and simpler than cure.
Professor Russell Viner 
President
The Royal College of Paediatrics and Child Health (RCPCH)
Tel: +44 (0)20 7092 6000