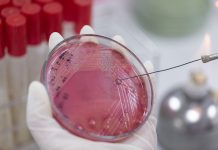
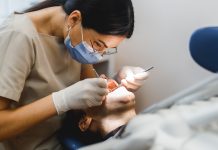
Experts Diane Bunn, Ellice Parkinson and Lee Hooper discuss the problem of dehydration particularly in care homes, first of all asking us to grab a coffee, tea, water, or juice before reading on…
Low-intake dehydration, when we don’t drink enough to remain healthy, is a common problem for older people all over the world; it is an even greater problem for those receiving care – whether living at home, in long-term care facilities or hospitals. Risk of low-intake dehydration increases with older age and develops more quickly, due to physiological, physical, social and cognitive changes.
In everyday living, obligatory fluid losses (through urine, faeces, sweating and breathing) need replacing, otherwise, dehydration occurs. Dehydration is strongly associated with poor health outcomes, including functional decline, increased risk of hospital admission and mortality. (1) The physiological processes of ageing which increase older people’s risk of developing dehydration include:
• Reduced sensitivity of the thirst response to dehydration (not feeling thirsty, even though the body needs more fluid).
• Reduced renal concentrating capacity (so that more, dilute urine is produced, and more fluid is lost.)
• Reduced muscle mass (reducing the amount of water stored in the body).
Physically, there is increased likelihood of functional impairments, making accessing drinks more difficult, and for those with cognitive impairments, remembering to drink may be an issue as well as incorrectly thinking that they may have had a recent drink. As if this plethora of issues was not enough, there are social and behavioural reasons why older people may not drink well. Many older people restrict their fluid intake to reduce toilet visits, without understanding the associated dehydration risk. Relying on carers (family or domiciliary workers) to provide drinks means that the timing and choice of drinks and the drinking vessel may not always meet personal preferences, reducing enjoyment and independence in drinking. If help is required with maintaining continence, then there may be extra work for their carers if having an extra drink.
Drinking is a social bonding activity – when we drink with others it creates belonging. But with increasing age, social contacts can reduce, so social cues to drink, and the satisfaction associated with drinking, also disappear. Finally, older people are often unaware of their changing hydration needs, and how, when and what adjustments may be appropriate to support hydration for healthy ageing. (2)
What does this tell us about how to support older people to drink well and prevent low-intake dehydration?
Supporting older people to drink well
Developing good drinking habits can help support hydration. Good habits include drinking regularly throughout the day, making drinking more enjoyable, by making drinking into a social occasion, and making sure that preferred drinks are served. Talking with older people to explore worries and fears around drinking can increase awareness about the need to drink (even if not feeling thirsty) and identify (and remedy) barriers to drinking.
Hydration care for older people living in care homes
For older people reliant on others to meet their hydration needs, carers also need support in recognising and developing hydration needs of the people they care for. We have undertaken a number of studies in UK care homes to provide an evidence-based approach to supporting hydration care in care homes.
Dehydration Recognition in our Elders (DRIE)
A key element of hydration care is recognising when dehydration is occurring. Health and social care professionals have always relied on signs and symptoms of dehydration (e.g., thirst, dry mouth, dry skin, dark urine, reduced skin turgor etc) and recommendations to use these are found in many nursing and medical textbooks. However, how do we know that these signs and symptoms correctly identify dehydration in peopled aged over 65 years?”
To answer this, we assessed a range of signs of dehydration in 188 care home residents and compared findings with serum osmolality, the definitive dehydration test. We found the commonly-used symptoms to be unreliable in detecting dehydration, and recommend that they be withdrawn from use. (3-5) Instead, we recommend a care home approach to supporting drinking for everyone to embed drinking and support for drinking within the care home culture. (6)
Conclusions
Low-intake dehydration, not drinking enough, is a serious and common problem for ageing adults. Looking forward, increased life expectancy and increasing numbers of people reaching older ages means that we need to better understand more fully how we can support older people to meet their hydration care needs, as a means of promoting health and wellbeing and maximising healthy years without disease, tailoring interventions and public health messages accordingly. (7) Public messaging tends to focus on the needs of all adults, rather than the specific needs of older adults, as well as tending to focus on nutrition more generally, rather than hydration specifically.
Much more research is needed in this area, to understand how best to develop effective public health messaging aimed at older adults and those approaching advancing years, around the importance of drinking to prevent low-intake dehydration and its association with poor health outcomes. For many, often those who have freedom of choice in deciding what, where, when and how to drink, the solution is obvious – we need to make sure favourite drinks and the appropriate support are available, facilitating and valuing pleasurable social contacts as essential support for drinking.
However, this oversimplifies the issues and doesn’t recognise more complex underpinning reasons of why older adults may not be drinking enough, and we need to explore this further to develop evidence-based effective hydration care measures, working with older adults (and their carers) to do this. It is highly likely that dehydration has increased during the COVID-19 pandemic, as older adults, whether living at home or in care homes, have been isolated and experienced reduced social contact. We all need to build back our social contacts, and remember to enjoy a drink together when we do socialise.
We hope you enjoyed your drink whilst reading this – now it’s time for another…
We would like to acknowledge the support of National Institute for Health Research (NIHR) developed network ENRICH (Enabling Research in Care Homes), who have provided support and guidance for the research team and care homes who have participated in our research into hydration care.
References
- Hooper L, Bunn D, Jimoh F, Fairweather-Tait S. Water-loss dehydration and aging. Mech Ageing Dev [Internet]. 2014 Dec [cited 2013 Dec 16];136–137:50–8. Available from: http://linkinghub.elsevier.com/retrieve/pii/S0047637413001280
- Pettigrew S, Pescud M, Donovan RJ. Older people ’ s diet-related beliefs and behaviours : Intervention implications. Nutr Diet. 2012;69:260–4.
- Bunn DK, Hooper L. Signs and Symptoms of Low-Intake Dehydration Do Not Work in Older Care Home Residents – DRIE Diagnostic Accuracy Study. J Am Med Dir Assoc [Internet]. 2019; Available from: https://doi.org/10.1016/j.jamda.2019.01.122
- Bunn D, Jimoh F, Karrouzze I, K W, Hooper L. Effective hydration care for older people living in care homes. Nurs Tiimes. 2019;115(10):54–8.
- Jimoh OF, Brown TJ, Bunn D, Hooper L. Beverage Intake and Drinking Patterns — Clues to Support Older People Living in Long-Term Care to Drink Well : DRIE and FISE Studies. Nutrients. 2019;11(2):pii: E447.
- Bunn D. UEA Hydrate Group: DrinKit [Internet]. DrinKit. 2019 [cited 2021 Aug 27]. Available from: https://www.uea.ac.uk/web/groups-and-centres/uea-hydrate-group/drinkit
- Kingston A, Wohland P, Wittenberg R, Robinson L, Brayne C, Matthews F, et al. Is late-life dependency increasing or not? A comparison of the Cognitive Function and Ageing Studies (CFAS). Lancet, 2017.
Contributor Profile
Contributor Profile
Contributor Profile
Editor's Recommended Articles
-
Must Read >> Dehydration in health and social care