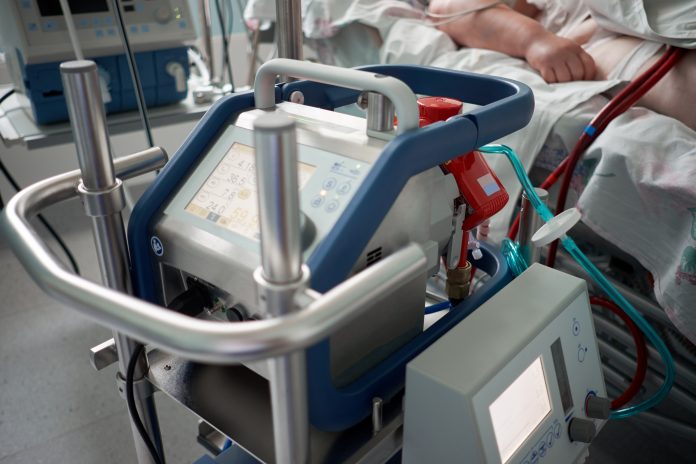
According to data collected by 400 healthcare professionals at the worst moment of the US outbreak, the life support machine that acts in place of the heart and lungs is crucial to reducing COVID-19 deaths for the critically ill
The study was conducted by physician-researchers at Beth Israel Deaconess Medical Center (BIDMC) and Brigham and Women’s Hospital (BWH), with the help of 400 grassroots professionals who collected crucial data at the height of the US outbreak.
This data shows that there is new evidence on how well ECMO machines work to save critically ill patients. This is the first study of its kind.
Firstly, what is an ECMO machine? Why isn’t everyone using it?
The public is by now, well-aware of what a ventilator machine is. They help those with impaired lungs to continue breathing, a device that Prime Minister Boris Johnson was rumoured to have needed during his personal experience with COVID-19.
However, what happens when lungs are too injured for even a ventilator?
Extracorporeal membrane oxygenation (ECMO) does the work of the lungs by removing carbon dioxide and adding oxygen to blood – outside the body. The ECMO machine can then become the dividing line between which critically ill patients live and die. Before this pandemic created intensive lung and heart problems, these machines were more commonly used for newborn babies.
For the second question, unfortunately, the procedure is intensively expensive. An ECMO machine must be run in ICU, and continuously monitored. Rough charges for ECMO in 2014 were around $550,000.
“ECMO gives patients’ lungs time to heal when we’ve exhausted every other aspect of care for these patients – it can be a bridge to recovery,” said corresponding author Shahzad Shaefi, MD, Co-Director of the ECMO Program at BIDMC and in the Department of Anesthesia, Critical Care and Pain Medicine.
“But ECMO’s efficacy in the context of COVID-19 remains unclear. This work sheds new light on that question in the most robust way possible during the COVID-19 pandemic.”
‘The best data we have about critically ill patients’
“These findings are not only statistically significant, but very clinically meaningful,” said senior author David E. Leaf, MD, Director of Clinical and Translational Research in Acute Kidney Injury in the Division of Renal Medicine at the Brigham. “They show a considerable magnitude of benefit with ECMO – a 45 percent reduction in death – among the sickest patients. That’s very compelling evidence that ECMO saves lives.”
“This was a remarkable grassroots effort involving more than 400 research assistants, medical students, residents, fellows, and attendings across the United States collecting this data manually during the height of the pandemic. People were highly motivated to get this database assembled, as it represents the best data we have about critically ill patients with COVID-19 in this country.”
The team analysed data across ICUs in 68 hospitals in the United States, an effort led by Doctor Leaf. The resultant STOP-COVID dataset includes more than 5,000 critically ill adult patients and depended on a dedicated volunteer workforce to collect more than 800 individual data elements per patient, all by manual chart review.
3% of critically ill patients received ECMO treatment
Overall, the scientists found that 190 of the 5,122 critically ill adults (3%) admitted to the ICU with COVID-19 between March 1 and July 1, 2020, received treatment with ECMO. Among those 190 patients, nearly 70% survived to hospital discharge or at least 60 days following ICU admission.
Target trial emulation is analytic technique which lets researchers use observational data to infer causality – when randomised controlled trials are unavailable. This is perfect for ongoing tragedies that have no time to be lab-tested when they still need to be treated.
Using this strategy, the team found that patient treated with ECMO in the first seven days of ICU admission had a considerable reduction in mortality compared to those who were similarly ill without ECMO. Specifically, among the 1,297 patients eligible for the target trial emulation, just over a third of the 130 who received ECMO died, compared to nearly half of those who did not receive ECMO.
‘Are we saving lives?’
“The real question with ECMO is, are we saving lives, or – candidly – are we prolonging poor outcomes and death,” said Shaefi, who is also Assistant Professor in Anesthesia at Harvard Medical School.
“The benefit of ECMO prevailed across all of our analyses. In the absence of a randomized controlled trial, which traditionally been very difficult to cleanly do in ECMO, this work represents perhaps the best current evidence we have of the role of ECMO in treating select critically ill COVID 19 patients.”