According to the American College of Surgeons, trauma informed care can help to “break the cycle of violence” – surgeons are usually the first healthcare professional to treat victims of violence
The role of a surgeon extends beyond caring for an injury. The ACS have created a four point strategy for helping victims of violence to break their cycles – an issue that has increased over the economically and socially tumultuous pandemic, as root causes of violence amplified.
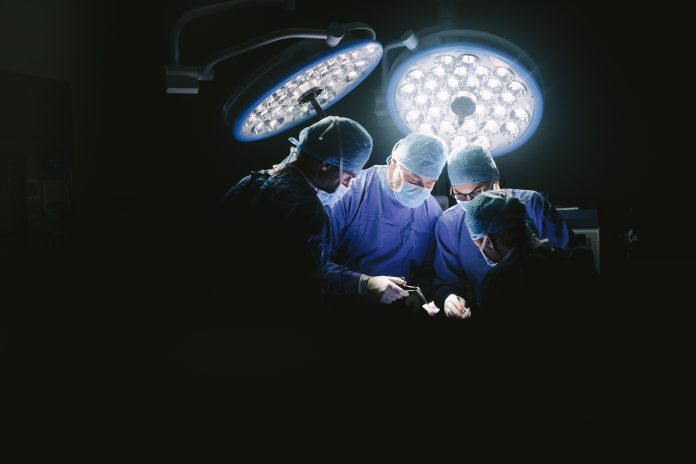
Sometimes, the first person in the healthcare system to speak with a victim of violence is the trauma surgeon. In Emergency rooms across the US, surgeons ask quick, gentle questions to establish the extent of damage to a human. They are treating physical damage, but it is intertwined with psychological damage.
“Physical trauma leads to psychological trauma and psychological trauma predisposes to physical trauma. Optimally addressing one, requires addressing the other,” said the ACS.
The ACS Improving Social Determinants to Attenuate Violence (ISAVE) workgroup say that Trauma centres can help address root causes of violence, improve health, and reduce inequities in marginalised communities.
What are the four strategies to “break the cycle of violence”?
- Development and Implementation of Trauma Informed Care in All Trauma Centres
- Integrating Social Care into Trauma Care
- The Trauma Centre’s Role in Investing in At-Risk Communities
- Advocacy
“Violence, in and of itself, is very much the end result of social determinants of health, structural racism, and structural barriers in our country that have existed for a long time,” said Rochelle A. Dicker, MD, FACS, of the division of trauma and critical care, University of California at Los Angeles Geffen School of Medicine.
“The strategies we propose are very action-oriented. Trauma is not just about the physical injury but has a broader definition. We need to be more comprehensive and aware of that as we treat our patients.”
‘Hospitals investing in their communities’ creates support
“It is important that people have access to trauma centers, but the other piece is hospitals investing in their communities,” Dr. Dicker said. “For example, putting in place vocational training programs so that the community is part of the employment process in a hospital itself. Also, whether the hospital uses local vendors for food; that’s an investment in the local community.
“Investment truly is the ability to put dollars into the communities that are in such great need.”
‘We are all in this together’ say authors
Health and wealth are inextricably tied to one another. For some, trauma can also be a generational experience.
The authors further said: “Black and Brown communities suffer heavily from a racial wealth gap relative to white communities, although rural white Americans are also deeply impacted by this gap and share a common lack of access to mechanisms to build financial security.
“Creating opportunities for financial and educational inclusion may not be seen on the surface as a health-related matter but, in fact, it is at its core.
“Although complex, effective interventions for violence are not as complex as those required to combat a novel corona virus pandemic, and as the COVID-19 pandemic has plainly demonstrated, we are all in this together. What affects one of us, affects all of us.”