The Centre for Lactation, Infant Feeding and Translation (LIFT) at Swansea University seeks to better support families in feeding their baby
How a baby is fed can feel like one of the most important but overwhelming decisions new parents make. Many mothers want to breastfeed, but the UK has some of the lowest breastfeeding rates in the world, which are still declining. Although over 80% of mothers start breastfeeding, many stop in the early weeks, often before they are ready due to not getting the support that they need – but the benefits of breastfeeding need to be highlighted.
We know that on a population level, breastfeeding protects infant and maternal health. Babies who are breastfed have a lower risk of infectious disease and breastfeeding lowers maternal risk of reproductive cancers, heart disease and diabetes. Additionally, there are economic and environmental reasons to protect breastfeeding. However, our research shows that how a baby is fed can also have a long-lasting impact upon maternal mental health.
Although formula milk can support babies when they cannot be breastfed, this doesn’t always fix the broader impact for women of not being able to breastfeed. The benefits of breastfeeding can also be important for religious or cultural reasons. It might be a preferred way of comforting and connecting with her baby, particularly after a traumatic birth. Breastfeeding is also about women’s reproductive health and a failure to support breastfeeding conveys the message that women’s health does not matter. As a result, we hear many stories of regret, anger and grief decades after women were unable to breastfeed.
Just because breastfeeding is a biological norm, that doesn’t make it easy
The question arises as to why many women struggle with breastfeeding and our research over the last decade shows the complexity of this. Just because breastfeeding is a biological norm, that doesn’t make it easy and breastfeeding works best when women are part of a culture that is supportive of breastfeeding. However, we lost much of our breastfeeding knowledge and skill when formula milk was promoted as superior to breastfeeding during the 1950s and following decades. Formula became our norm, heavily influenced by industry messaging undermining the benefits of breastfeeding. Despite breastfeeding being encouraged antenatally, a lack of government investment in research and expertise to support breastfeeding and parents in general means that many women are struggling to get the practical and emotional support that they need.
Our research and collaboration with governments, public health bodies and infant feeding charities seeks to create an environment that doesn’t simply promote breastfeeding but protects and supports it. This involves campaigns around understanding breastfeeding and normal baby behaviour, highlighting the importance of breastfeeding for mental health, and calling for greater investment into supporting all types of infant feeding.
Human milk is lifesaving for premature babies. When they cannot receive their own mother’s breastmilk, specially heat-treated donor milk from other mothers who have been carefully screened can protect their health and development. Recent WHO recommendations are that donor milk should be available for all preterm babies where there is a shortfall of maternal milk.
The impact of donor milk and wellbeing
As part of this, we have been exploring the impact of donor milk in protecting wellbeing, through supporting parental mental health and providing a bridge for mothers to establish their own lactation. Our collaborative data shows that when mothers who are unable to breastfeed for health reasons can access donor milk for their baby their anxiety and depression scores significantly decrease. Exploring why this might happen, our research suggests that it is the reassurance of accessing human milk for their baby but also the broader experience of being listened to, supported and feeding choices being respected.
However, until recently, Wales was the only country in the UK without its own donor milk bank. Donor milk was brought in from England to support babies in neonatal care but due to logistical reasons women in South, West and Mid Wales struggled to donate their milk as they lived too far away from a milk bank. Working with the Human Milk Foundation (HMF) a charity dedicated to ensuring equitable and assured access to donor human milk, Blood Bikes Wales who provide a free courier service for the NHS, and Swansea Bay University Health Board we established a donor milk hub in Swansea supported by Research Wales Innovation funding from HEFCW. The hub stores treated donor milk for use on neonatal wards and enables local mothers to donate their milk. Our novel research with donors already shows how protective the act of donation can be, helping them to feel part of a community and that they are making a difference in supporting other families.
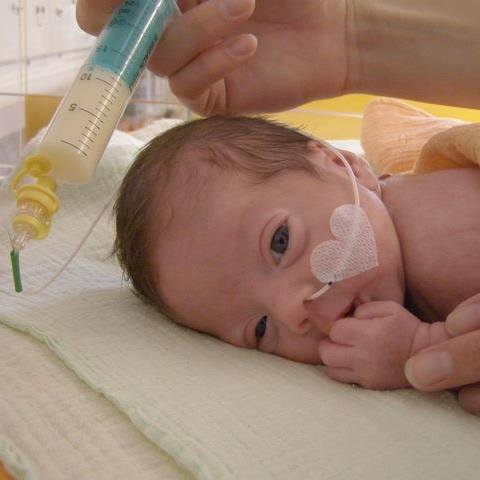
Increasing access to donor milk
At present, donor milk is typically rationed for babies born under 32 weeks but alongside providing donor milk to hospitals through the Hearts Milk Bank the HMF supports families to receive donor milk for their baby, when they would not usually be eligible, funded through charitable and research funding. This includes mothers who are undergoing cancer treatment or another health issue that prevents them from breastfeeding or establishing a full supply.
The goal of our research at LIFT is to ensure that all parents feel informed and supported however they want to feed their baby. Donor milk plays an important role in that, and as services scale, government support is needed to meet the growing demand across the UK milk bank network. Our collaborative network is committed to ensuring nationally equitable milk banking services that can create the broadest range of public health impacts for future generations.

This work is licensed under Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International.


