Marco Landi, President of Council of European Dentists, considers dentistry during the COVID-19 pandemic and the extent to which oral health is still a priority
The COVID-19 pandemic continues to have devastating health, social and economic consequences and is profoundly affecting the delivery of health services, including dentistry. During the early stages of the public health crisis, the provision of oral care in Europe was significantly curtailed. European governments recommended that dentists postpone elective dental procedures and provide emergency-only dental treatments, both to prevent the spread of infections and to keep dental patients from burdening hospital emergency departments. This approach not only fed the patients’ fears of contracting the virus when visiting the dentist, but it also seemed to confirm the image of oral care as an optional luxury rather than a necessity.
Importance of oral health promotion
Neglecting oral health of course predates the COVID-19 era, even though oral conditions are commonplace across the globe. The 2017 Global Burden of Disease Study, which is considered to be the definitive research project on sources of mortality and disability, estimated that oral diseases affect close to 3.5 billion people worldwide, with untreated dental caries (tooth decay) in permanent teeth being the most common health condition.
However, it was only in 2019 that the World Health Organization finally included oral health in the Political Declaration on Universal Health Coverage, eight years after the United Nations High-Level Meeting on Noncommunicable Diseases recognised that oral diseases pose a major health burden for many countries.
COVID-19 and oral health inequalities
The prevalence of oral diseases, which share common factors with other major non-communicable diseases, continues to increase in Europe. This is primarily due to the use of tobacco and alcohol, excessive sugar consumption, and other lifestyle factors, as well as to poor access to oral health services, particularly for weaker socioeconomic groups. Many of these factors have been heightened during the pandemic. Unless we act now, this will lead not only to poorer oral health outcomes but to impaired general health across the board.
The current public health crisis is deepening oral health disparities in access to care. This is due to different factors, including insufficient funding for national health budgets, lack of prevention campaigns aimed at general and specific health targets, and absence of new legislative programmes oriented towards promoting and safeguarding a healthy lifestyle. In addition, we are failing to prioritise fragile and vulnerable population groups that already have limited access to regular check-ups meant to detect oral diseases, as well as early signs of general health issues, such as oral cancer, diabetes, lymphoma and cardiovascular diseases. Not by coincidence, it is exactly these groups with limited access to general and oral healthcare who are also at high risk for COVID-19.
Safety of dentistry during the pandemic
At the beginning of the COVID-19 pandemic, dentists were commonly considered among those occupations at the highest risk for COVID-19, due to the potential direct and indirect exposure to infectious materials. However, dentists have been practising strict infection control measures and taking universal precautions for
the last 50 years. There is growing evidence that dentistry remains safe for dental patients, members of the dental team and dentists themselves also under COVID-19 conditions. Effective personal protective equipment is applied to protect both the dental personnel and the patient, and appropriate protocols are followed, which allows the dental team to perform oral care procedures in a safe environment.
In most European countries, dental practices began slowly reopening in spring and summer 2020, with constantly updated guidance on the safety procedures required. International, European and national bodies published various recommendations, sometimes contradictory and wrongly interpreted. In November 2020, the Council of European Dentists published its own statements on the safety of dentistry and on effective dental educations in COVID-19 times, strongly recommending the continuity of oral care provision during the pandemic.
Oral hygiene during a pandemic
Brushing your teeth is crucial, even during a pandemic, in the view of the Swiss Dental Association (SSO). This approach to oral hygiene is not only to keep your teeth healthy, for example, but parents should also check that their children brush their teeth at least twice a day in a careful manner. “All it takes is a soft children’s toothbrush and a Children’s toothpaste containing fluoride,” according to the SSO.(1)
Taking Switzerland as a case study, it is interesting to note that dental treatments were approved again there in April 2020 despite WHO recommendations to postpone non-urgent dental treatments because of COVID-19. SSO believes that “official recommendations at national, regional and local level are to be applied” and as such, the Association of Cantonal Dentists of Switzerland (VKZS) with SSO recommended “a comprehensive protection concept” that is appropriate to minimise the risk of transmission during dental procedures.
The hygiene measures in place are based on scientific knowledge and SSO President, Dr Jean-Philippe Haesler stressed that the health of your mouth and teeth are important, and play a vital part in the overall state our health. “It is therefore essential that the patients can be treated according to their needs to prevent tooth damage. Patients in Switzerland can trust that…dentists professionally implement protective measures before and during treatment. Dental practices in Switzerland are safe.”(2)
The information above concerning oral hygiene during a pandemic was compiled by the Editor of Open Access Government during December 2020.
COVID-19 as an opportunity to refocus oral care
The COVID-19 pandemic presents an overarching opportunity to rethink the future of dentistry and address pressing issues faced by the field, rather than going back to business as usual.
Current circumstances provide a chance to reorient oral care towards a less invasive and more preventive approach, an endeavour which tackles the shared risks for oral diseases and other non-communicable, and embraces the non-surgical approach to caries management, as promoted by the Council of European Dentists in our White Paper on prevention. By focusing on the reduction of risk factors and promotion of a healthy lifestyle in community settings, as well as on increasing access to oral health, we propose to shift the dental care paradigm from treatment to prevention. These methods present a major opportunity to expand the access to preventive and restorative care for vulnerable populations, but they must be combined with policy changes, sustainable payment reform, and changes in the education of oral health professionals.
Health in the European context
In this context, the Council of European Dentists welcomes what seems to be a change of pace in European health policies, with more importance attributed to health in the European Commission’s work, with a bold EU4Health Programme and multiyear budget proposals. These initiatives aim to strengthen national health systems so that they can face epidemics as well as long-term challenges by stimulating disease prevention and health promotion, the digital transformation of health systems and increasing access to healthcare for vulnerable groups. The European Commissioner for Health’s approach and priorities to work on urgent health issues such as the fight against cancer, reducing the number of antimicrobial-resistant infections and improving vaccination rates is an important step forward in building strong and resilient health systems all over Europe.

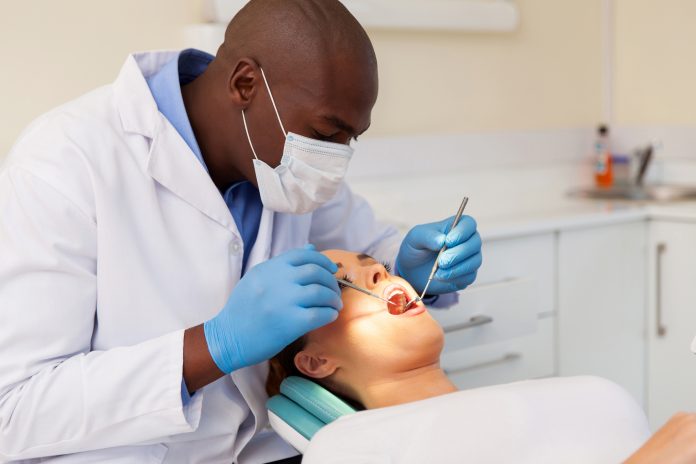










As a dentist, i realize i am a bit biased, but I have seen the devastating consequences of neglecting dental hygiene as well as necessary procedures and maintenance. With dental clinics already having such high standards of sanitation, I believe there is little to no risk for them to remain open, and certainly negative health consequences.