Maria Piggin, Chair of PNH Support tells us about the rare disease, paroxysmal nocturnal haemoglobinuria (PNH) and in this area, collaborations for change
Paroxysmal nocturnal haemoglobinuria (PNH) is a rare disease affecting between approximately one and two people in every one million and affects both men and women at different ages. PNH is an ‘acquired’ genetic disease, so it cannot be inherited and patients are usually diagnosed in young adulthood.
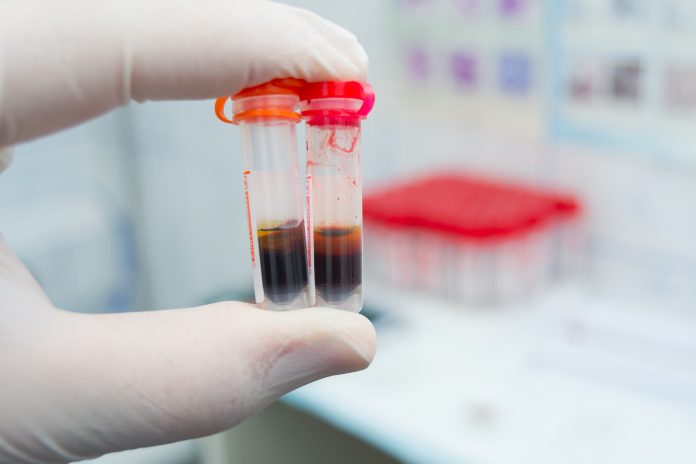
PNH is a bone marrow failure disorder where abnormal blood cells can emerge from the bone marrow lacking multiple GPI- anchored proteins as a result of a genetic defect (mutation) in the “PIGA” gene. Absence of these proteins leave the blood cells unprotected against a series of complex reactions called “complement activation” which is part of the body’s normal immune response to fight infections. As a result, the red blood cells are destroyed (haemolysis) which is the main cause of PNH symptoms and complications.
Treatment
PNH is often diagnosed with aplastic anaemia although patients can have one without the other. Treatment for aplastic anaemia is different from PNH and will depend on whether it is inherited or acquired.
Since June 2007, there has been a licenced treatment for PNH in Europe. This treatment blocks the complement part of the immune system. It is not curative but dramatically reduces symptoms, the most significant of which is the occurrence of blood clots (which used to be the main cause of death in patients) and allows patients to have the life expectancy of someone without PNH. It has also more recently been used safely in pregnancy, which previously had to be avoided by PNH patients due to the risk of blood clots.
Although available in approximately 40 countries, unfortunately, this treatment is not available to all PNH patients globally due to its very high cost (approximately £300,000 per person per year). Bone marrow transplants can cure PNH but are rarely used due to the risk of severe complications.
Despite the fact that PNH patients who have access to treatment are in an enviable position, the “diagnostic odyssey” which affects rare diseases generally, equally applies to PNH. GPs and haematologists need to be able to recognise a disparate set of symptoms, such as anaemia, stomach and back pain, dysphagia (difficulty swallowing), jaundice, breathlessness, erectile dysfunction, severe fatigue and dark or red coloured urine. As not all patients experience all these symptoms and especially, perhaps the most telling one, dark/red coloured urine, the recurrent stomach pain can send patients down a urology and/or gastroenterology pathway for years at a time. Anorexia has been another misdiagnosis resulting from weight loss due to difficulty swallowing as a result of the dysphagia (which results from the free haemoglobin from the damaged red cells binding and removing nitric oxide). Complications caused by PNH prior to diagnosis can lead to irreparable damage which is why diagnosis and/or referral to a PNH specialist in a timely manner, is vital.
Diagnosis
The diagnosis process would benefit significantly from a multidisciplinary approach by the medical profession as well as timely referrals by haematologists to the PNH National Service (a specialised service) commissioned directly by NHS England) based out of both St James’s Teaching Hospital in Leeds and Kings College Hospital in London. These hospitals are global centres of excellence for PNH and it was thanks to Professor Peter Hillmen’s research which led to the approval of the currently licenced treatment and as a result, a transformation in PNH patients’ quality (and length) of life.
PNH Support is a Charitable Incorporated Organisation established in 2015 by patients for those living with PNH (and their families) in England, Wales and Northern Ireland and run by volunteers. Scotland has its own group, PNH Scotland.
One of the primary drivers for setting up PNH Support was the need for an independent, legal platform through which PNH patients could engage with their many stakeholders including pharmaceutical companies undertaking continuing research and development into PNH, the NHS, homecare providers, the National Institute for Health and Social Care Excellence (NICE), the European Medicines Agency and other patient organisations both locally and internationally.
Peer-to-peer support
Of equal importance to the formation of PNH Support, was the need for a platform through which peer-to-peer support could be facilitated as it was very common for patients to never have spoken to another patient, which can be extremely isolating. PNH Support holds regional patient meetings, a biennial patient and family conference and moderates a closed Facebook group. The sharing of experiences with someone who understands, cannot be replaced.
The need to share information, common challenges, joint approaches and leverage combined numbers was a motivation in the recent creation of the PNH Global Alliance comprising PNH patient organisations from Europe, Russia and Canada. It is anticipated that this alliance will only grow to include other countries in the near future.
In the face of an impending exit from the European Union and the loss of membership by UK clinicians from European Reference Networks (ERNs), forging homegrown networks is ever more important for collaboration and knowledge sharing especially in rare diseases. For this reason, “Together for Healthy Marrow” was recently formed comprising patient organisations for the following acquired and inherited rare bone marrow failure disorders: PNH, Aplastic Anaemia, Fanconi Anaemia, Dyskeratosis Congenita and Diamond Blackfan Anaemia.
PNH Support has benefitted enormously from the knowledge and experience of European patient advocates especially those in the HIV and oncology communities. Significant challenges remain for rare disease patient advocates where independence and credibility are paramount whilst engaging with their commercial and regulatory stakeholders. Rare disease communities (with fewer numbers to begin with) have even fewer advocates with the health, time, capacity and knowledge to undertake the advocacy required to engage meaningfully with all relevant stakeholders.
The European Patients’ Academy for Therapeutic Innovation (EUPATI) has done a valiant job since 2014 to train in excess of 150 patient advocates from across Europe in a variety of disease areas and is currently crowdfunding to train more. EUPATI also developed a “toolbox” of resources, case studies and guidance documents for training patients and industry about involving patients in research and development. These are all widely accessible under a creative commons licence.
Patient involvement
“Patient involvement” in publicly funded research has been a requirement of the National Institute for Health Research’s INVOLVE since 1996. Pharmaceutical companies are fairly new to the concept and value of this kind of involvement which they (and our European colleagues) refer to as “patient engagement”. Leaving aside definitions, the principle of reciprocity and partnership is key. Patients, even more so in the rare disease space, are the best (and only) people to inform researchers of their ‘unmet needs’. They know what research is a priority for them, what kind of trial design is going to appeal to potential participants, what study outcome measures are important to them, particularly, the relevance of Patient Reported Outcome Measures (PROMs), which are increasingly being developed for specific disease areas. PROMs identify how patients’ experience a particular treatment rather than how their body reacts to it which is what is frequently measured in a clinical trial. Patients are integrally important in the research and development process from identification of the unmet need to engaging in processes with regulators and health technology assessment agencies. The collaboration and sharing of knowledge between even small patient organisations facilitate ‘activated‘ patients to play a part in the development of more effective and patient relevant treatment options.