Researchers from the University of North Carolina and NC State have developed artificial beta cells that automatically release insulin into the bloodstream when glucose levels rise, leading the way for new diabetes treatment
At least six million people in the United States use insulin as a diabetes treatment, either by injection or a mechanical pump, but a major problem with current insulin treatments, however, is that they can’t control blood glucose levels automatically and efficiently.
Artificial beta cells (ABCs)
The artificial beta cells (ABCs) are much more patient-friendly and mimic the functions of the body’s natural glucose-controllers. The idea is that the AβCs could be subcutaneously inserted into patients, which would be replaced every few days, or by a painless and disposable skin patch.
The ABCs are constructed with a simplified version of a normal cell’s two-layered lipid membrane. The key innovation is what these cells contain: specially designed, insulin-stuffed vesicles. A rise in blood glucose levels leads to chemical changes in the vesicle coating, causing the vesicles to start fusing with the ABC’s outer membrane – thus releasing the insulin payloads.
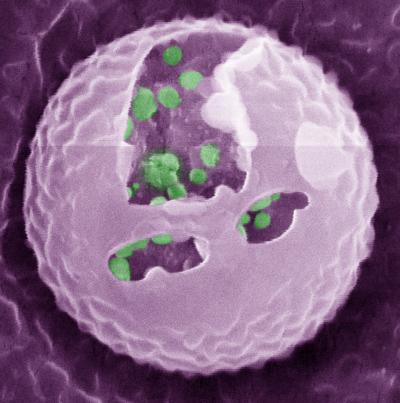
The study
The researchers reported, in the Nature Chemical Biology journal, that a single injection of the ABCs into diabetic mice quickly normalised the animals’ blood glucose levels and kept them normal for up to five days.
Principal investigator Zhen Gu, PhD, a professor in the Joint UNC/NC State Department of Biomedical Engineering said,”Our plan now is to further optimize and test these synthetic cells in larger animals, develop a skin patch delivery system for them, and ultimately test them in people with diabetes.”
“This is the first demonstration using such a vesicle fusion process for delivering insulin that employs insulin-containing vesicles like those found in a beta cell and can reproduce the beta cell’s functions in sensing glucose and responding with insulin ‘secretion’,” said Zhaowei Chen, PhD, a lead author and postdoctoral researcher in Gu’s lab.
Further testing
Co-author John Buse, MD, PhD, the Verne S. Caviness Distinguished Professor at UNC, chief of the division of endocrinology, and director of the UNC Diabetes Care Center, said, “There is still much work needed to optimize this artificial-cell approach before human studies are attempted, but these results so far are a remarkable, creative first step to a new way to solve the diabetes problem using chemical engineering as opposed to mechanical pumps or living transplants.”
The American Diabetes Association, the National Science Foundation, the National Institutes of Health, and the Alfred P. Sloan Foundation funded this research.
References