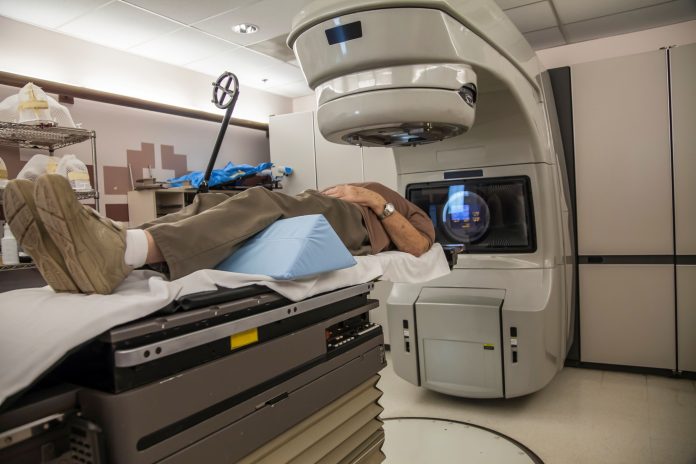
Adonis Sfera and Zisis Kozlakidis provide recent insights into cellular and biological pathways from studies on communicable diseases
The human body, with its complex networks of cellular and biological pathways, has evolved a large number of mechanisms to control the different imbalances that might arise. These imbalances, if remaining unchecked, can eventually manifest as non-communicable diseases, such as cancer, or as a result of communicable diseases, such as after infection by a virus such as SARS-CoV-2, causing COVID-19.
The intense study of the latter over recent years has resulted in the significant production of scientific knowledge for the immediate necessity of not only controlling the pandemic but also towards gaining a deeper understanding of existing cellular and biological pathways. It is anticipated that the recent discoveries will add to the existing body of knowledge and further facilitate the understanding of the link(s) between biological mechanisms and the development of different diseases, paving the way at the same time for the development of new treatments.
Here, we present only an indicative few of the recent COVID-19 derived discoveries and working hypotheses, as applied to the cellular mechanisms and their relevance for better understanding the mechanisms behind different clinical conditions.
Endothelial senescence, chronic fatigue syndrome and COVID-19
The first such example is Myalgic encephalomyelitis/ chronic fatigue syndrome, a serious illness of unknown cause. It is characterised by some or all of debilitating exhaustion, memory impairment, pain and sleep abnormalities.
According to the Centers for Disease Control and Prevention (CDC), it is estimated that in the US alone, 836,000 to 2.5 million Americans may be suffering from ME/CFS. Importantly, the majority of people with ME/CFS remain undiagnosed as there are no laboratory tests that can provide such a diagnosis. Thus, diagnosis takes place empirically, based on in-depth evaluation of a person’s symptoms and medical history by their treating clinicians. Viral infections are believed to initiate the pathogenesis of this syndrome although the definite proof remains elusive.
With the unfolding of COVID-19 pandemic, the interest in this condition has resurfaced as excessive tiredness, a major complaint of patients infected with the SARS- CoV-2 virus, often lingers for a long time, resulting in disability and poor life quality.
Long-lasting myalgia and exhaustion were reported in over 40% of COVID-19 patients during the first two waves of the pandemic. Indeed, as muscle cells express abundant angiotensin converting enzyme-2 (ACE-2), the virus likely exploits the myocytes, engendering disabling symptoms such as fatigue and weakness. For example, preclinical studies have demonstrated that SARS-CoV-2-upregulated angiotensin II (ANG II) disrupts the muscle cell autophagy, impairing both the metabolism and contractility (1).
However, aside from directly accessing the myocytes, this virus can induce myopathy, muscle weakness and atrophy indirectly by upregulating proinflammatory cytokines, such as interleukin 1 beta (IL-1β) and 6 (IL-6), C-reactive protein (CRP) and tumour necrosis factor (TNF). When persistent, exertional and unrelieved by rest, myopathy may gradually morph into ME/CFS (2). Thus, a pre-existing working hypothesis has been further enhanced due to the intensity of research into COVID-19.
Membrane fusion in neurodegenerative studies
Using a similar approach, inroads can be achieved in our current understanding for some of the neurodegenerative disorders. A growing body of epidemiological and research data has associated neurotropic viruses with accelerated brain ageing and increased risk of neurodegenerative disorders.
Many viruses replicate optimally in senescent cells, ie in cells that have stopped multiplying but don’t die off when they should, and as such they offer a hospitable microenvironment with persistently elevated cytosolic calcium, abundant intracellular iron and low interferon type I.
As cell-cell fusion is a major driver of cellular senescence, many viruses have developed the ability to promote this phenotype by forming syncytia, large multinucleated cells produced by two or more cells fusing. Cell-cell fusion is associated with immunosuppression mediated by phosphatidylserine externalisation that enable viruses to evade host defences. In hosts, virus-induced immune dysfunction and premature cellular senescence may predispose to neurodegenerative disorders.
This concept is supported by novel studies that found post-infectious cognitive dysfunction in several viral illnesses, including human immunodeficiency virus-1, herpes simplex virus-1 and SARS-CoV-2 (3). Therefore, the current strides in biological understanding should be able to elucidate pathways and clinical conditions well beyond the narrow research aims relating to the viral ability to infect cells and divert the normal functioning of the body towards the production of viral particles.
The pandemic could boost understanding of viruses
The current pandemic, caused by the SARS-CoV-2 virus, may be a catalyst for a better understanding of the role of viruses in the pathogenesis of many illnesses. As SARS-CoV-2 (and probably other viruses) utilise the molecular machinery involved in many different disorders, the clarification of these biological mechanisms may help with the development of better therapies.
Furthermore, by employing collaborative approaches from different clinical fields, conserved biological mechanisms can start to emerge, eventually being further investigated for potential drug targets.
Disclaimer
Where authors are identified as personnel of the International Agency for Research on Cancer/WHO, the authors alone are responsible for the views expressed in this article and they do not necessarily represent the decisions, policy or views of the International Agency for Research on Cancer/WHO.