In this exclusive guide to HRT, menopause specialist Dr Deborah Lee, Dr Fox Online Pharmacy, explores the ups and downs involved in deciding whether to start taking HRT
If you’re reading this, I hazard a guess you find yourself unsure about making a decision to take HRT. Take heart – you are by no means alone.
There are currently 11 million women in the UK aged 45 or over. The last 20 years have been a time of chaos, confusion and indecision for both menopausal women, people with wombs, and their health care providers. As a direct result, HRT prescribing fell by 50%. However, happily, confidence is returning and now HRT prescribing is definitely on the rise.
Menopausal symptoms can be severe and have a major, negative impact on quality of life. HRT is, without doubt, the most effective way to control these symptoms, but in the recent past, HRT usage fell by more than 80%, after the publication of two key research trials (WHI Study 2002, Million Women Study 2003). Public confidence in HRT was very low. But thankfully, things now look very different. Read on and find out more.
HRT is a safe, effective treatment for menopause
Here’s the good news! – HRT is indeed a safe and effective treatment. Menopause experts and statisticians have now carefully reanalysed these studies, reviewed the up-to-date medical evidence and come to this robust and reassuring conclusion.
These experts include the British Menopause Society, the Royal College of Obstetricians and Gynaecologists (RCOG), and The National Institute for Care and Health Excellence (NICE)
Any medication, not just HRT, carries some small risks, and before taking it you need a medical consultation. However, for fit, healthy women, who take HRT for 5 years to control menopausal symptoms, HRT is likely to convey benefit and not harm.
Whether you choose to take HRT or not, the most important issue is that you make your decision based on the correct facts. The pendulum has now swung in the opposite direction, and the health benefits of HRT should not be underestimated.
My aim in this article is not to reiterate the benefits and risks of HRT – which you can read elsewhere. It is to help you understand the factors, many of which are subconscious, which affect the HRT decision-making process. You will then be able to go into the HRT consultation with your provider from a balanced perspective.
By following the 7 steps of the decision-making process, you can then arrive at a decision with which you feel confident – whether or not you choose to go for HRT.
Don’t confuse HRT with the Pill
Don’t confuse HRT with the combined contraceptive pill. They are totally different products and the rules for prescribing each are very different.
HRT is just that – ‘hormone replacement’ – providing a low dose, natural (not synthetic) oestrogen, to replace the oestrogen your ovaries are no longer making.
The menopause struggle
If you are living through your own menopause experience right now, you may feel you are between a rock and a hard place. Many women and those with wombs have such a terrible experience at menopause, they feel like their whole lives are falling apart.
Lack of sleep, hot flashes, mental fatigue, mood swings/irritability, vaginal dryness, low libido and sexual problems are all too common. This all impinges on relationships, family life and the work environment. You become exhausted, emotional and anxious. Many women arrive at the clinic and burst into tears.
The big question then raises its ugly head – Should you, or should you not, take HRT?
There has been so much media hype suggesting that ‘HRT may be dangerous.’ That it ‘causes cancer,’ and ‘should be avoided at all costs.’ It can be very frightening to feel that nothing will change, the daily struggle with your menopause will just continue unabated unless you ‘give -in’ and take something (HRT) you feel pretty much uncertain about.
So, let’s explore the whole concept of how to make a decision about HRT – step by step.

The psychology of decision-making
Small decisions are easy to make. We make lots of these every day. However, more important decisions, which have bigger consequences, are a lot harder.
For example, if you are thinking of buying a house, and/or taking out a mortgage, you probably visited lots of properties, considered the pros and cons, imagined the ‘what-if’s’’ and then took financial advice, before you signed on the dotted line?
Decisions about health are no different – the principles are the same. When we make any decision, we are undertaking a series of thought processes. These eventually lead us to a belief, that we are now going to embark on the right course of action. Making a decision is a type of problem-solving.
To solve the problem, we need to know the facts. However, we will be considering these facts in the context of our own ideas, needs, preferences and personal, health care values.
To further muddy the waters, when you discuss these facts with your health care provider, they may very well have different ideas, needs, preferences and personal healthcare values to yours. How can these two ever meet in the middle?
When you arrive for your menopause appointment, if you have been suffering for some time with unpleasant menopausal symptoms, you may be in a state of emotional distress. Your thought patterns may be distorted – psychologists label this as being ‘irrational.’ Hence by virtue of the very condition itself, you may well not be in your best frame of mind, when having to make this HRT decision.
Emotional intelligence
We all have differing degrees of emotional intelligence (EQ) – this is a separate entity to our general level of intelligence (IQ). This can affect the whole process of making a decision.
Emotional intelligence is described as the ability to recognise your own emotions, and understand the emotions of others, in order to adjust your behaviour accordingly, and achieve the desired outcome.
Medical imaging has shown emotional intelligence to be associated with specific nerve pathways in the brain. People with lower levels of emotional intelligence find decision-making more difficult.
Lower levels of emotional intelligence are associated with depression, low self esteem, poor health choices and behaviour. Menopausal symptoms may also result in these outcomes. So many women arrive in the clinic at a disadvantage.
Emotional intelligence has a genetic cause. So, we can’t change it – but we can be aware of it and accept that it may influence the course of the decision-making process.
Factors affecting decision-making and taking HRT
The outcome of the decision will be affected by ‘unconscious bias.’ Examples and how these might affect the decision to take HRT, include:
- Repetition bias – The tendency to believe what you are told the most often. In recent years there have been a lot of damaging, and frankly fake news reports, about the dangers of HRT. The belief that HRT is dangerous – and causes breast cancer, will be in your subconscious mind before you even visit the doctor.
- Selection bias – People are prejudiced against new ideas and actively dismiss information they do not perceive as important. If a friend or family member had a bad experience on HRT, you may have subconsciously decided never to take HRT – as this has put you off.
- Peer pressure – The desire to conform to the group. If your friendship group, or work colleagues are all anti-HRT for whatever reason, there is a natural desire to conform and be like them.
- Underestimating uncertainty – People tend to feel they have more control over the future than they do. For example, you may be convinced that by eating healthily, you can beat the menopause and stay healthy, because eating is something you can control. The course of your symptoms is however something you cannot control.
- Anchoring – People are unwilling to shift a deeply help viewpoint owing to their belief in what they’ve been told previously. Call us stubborn, but once we’ve formed a viewpoint, we may be very resistant to change. You’ve been led to believe for a long time that HRT is not a good thing. It’s now difficult to reverse this viewpoint.
- Framing bias – Doctors often show you numbers, graphs and charts. To convey risk, it’s important not to have too much reliance on numbers. Look at pictorial guides and a variety of different tools. Don’t be afraid to say you don’t understand.
Understanding risk
One important point about decision-making, is to understand the concept of risk. Specifically, the difference between relative and absolute risk. The media twist statistics to create shocking headlines and sell news.
Understanding risk is very difficult, and we may not really get to grips with what we are being told. Perhaps we lack confidence, feel too embarrassed, or even feel too unwell, to ask the right questions.
Let’s put the risk issue as simply as possible. For example, if you read that using HRT increases your risk of breast cancer by 21%, you might be worried. A 21% increased risk sounds huge.
However, breast cancer is common in women not taking HRT.
- In women who have not used HRT – 27 out of 10,000 women aged 50-54, will be diagnosed with breast cancer in the next year. Breast cancer is a common cancer.
- A 21% increase in risk from the use of combined HRT users, brings the total number of breast cancers to 33 per 10,000. This means an extra 6 extra cases of breast cancer, per 10,000 women, per year in women using combined HRT.
Although this is still lamentable, 6 cases per 10,000 users, doesn’t sound nearly so bad. Especially when you realise that alcohol (drinking 2 glasses of wine per day) is also responsible for an additional 6 cases of breast cancer, and obesity, an extra 17 cases! Many women drink alcohol regularly and are overweight, and yet these risk factors are as bad for breast cancer risk as HRT, if not worse.
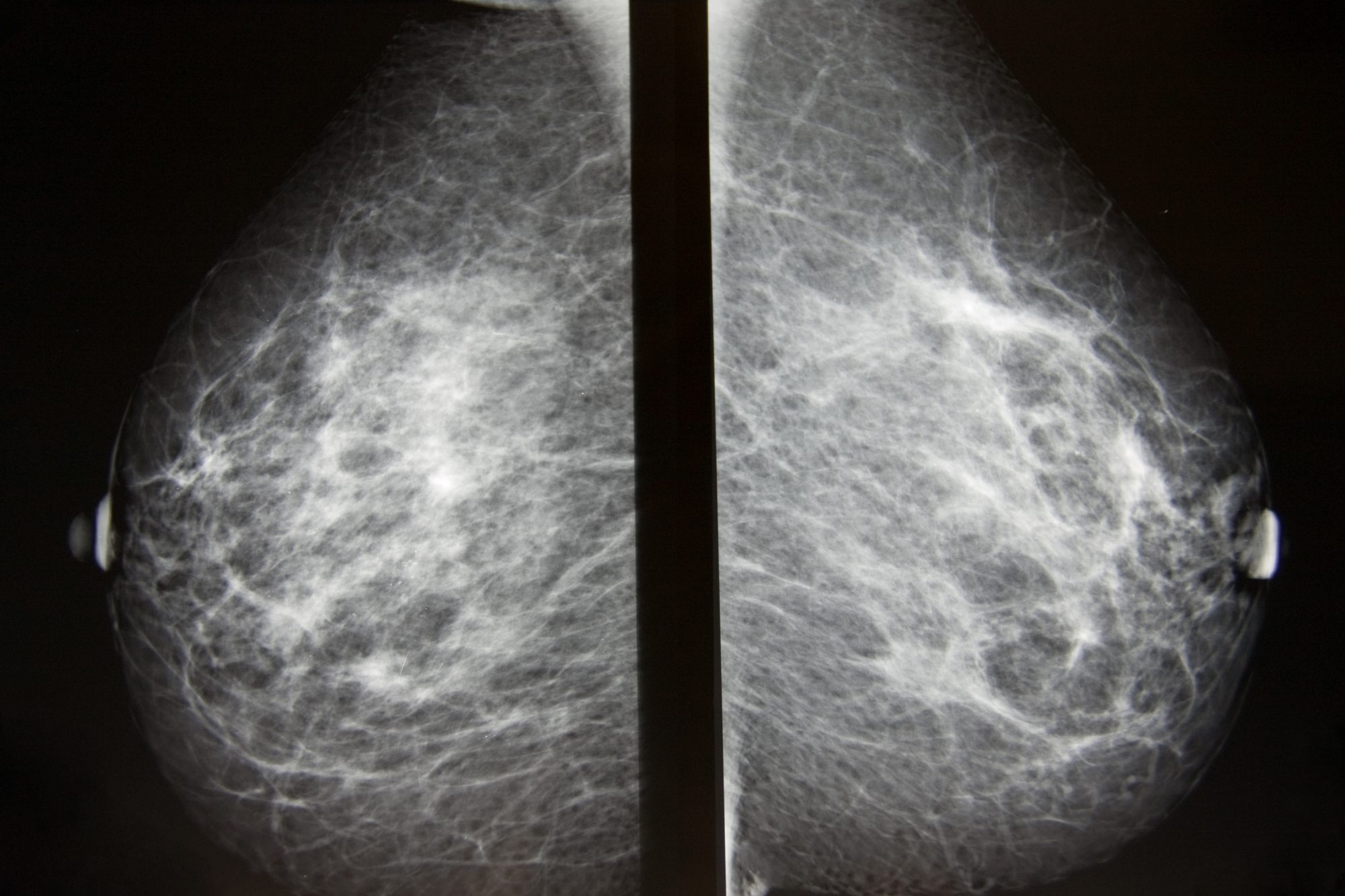
Breast cancer and HRT – a couple of important points
The additional risk of breast cancer from HRT, only applies to ‘combined HRT,’ that is women who take both hormones – oestrogen and progesterone.
If you have had a hysterectomy and hence, can take oestrogen-only HRT, this does not increase your risk of breast cancer. It may actually reduce it.
The increased risk of breast cancer in women who use HRT, only starts age 50. Under the age of 50, if you take HRT, you are no extra risk of breast cancer than you would be if your ovaries were working normally.
Decision-Making About Health Care Choices
There are various psychological models about the best decision-making processes, but all of them suggest a step-wise approach. For example:
Pam Brown, 2007 – ‘The 7 Steps of Decision-Making’
- Outline the goal and outcome
- Gather data
- Develop alternatives (i.e., brainstorming)
- List pros and cons of each alternative
- Make the decision
- Immediately take action to implement it
- Learn from and reflect on the decision
The seven Steps of a menopause consultation
Most of us are unaware that we come to the consultation with a whole host of unconscious bias (some are listed above). The doctor needs to also be aware of this. Try to overcome these biases by actively listening and being open to new ideas and suggestions.
Trust the medical staff to give you the most up to date information – they are all well trained and bound by their work codes of practice to give you the correct facts, from what is currently known.
Here is a list of steps to follow for the HRT consultation, based on Pam Brown’s model above.
- Why have you come to the clinic today? What specific symptoms do you have? What are you hoping to gain from your visit?
- Describe the symptoms you are suffering – and the way the menopause is affecting you.
- Discuss what options there are for treatment – HRT – and other options.
- Find out about the merits and disadvantages of each treatment. This will include a discussion about the risks and benefits of HRT.
- Decide which option to take – HRT or other. This may involve taking information home to think it over. It does not necessarily need to be made there and then.
- If you feel ready, and you have chosen HRT, decide on which type, tablet, patch or gel, which dose (low dose, standard dose, and higher dose) and how to use it.
- Go home and get started. Know when you need to be seen again, and what to do you when you need help or advice along the way. If you start HRT, this in usually in 3 months time.
Practical considerations
It’s a good idea to take a list of questions you want to ask to the clinic appointment with you. Also, don’t be afraid to write things down. You can ask for copies of fact sheets or information that are shown to you, to take home.
You are also entitled to have a copy of any medical letters written about you. This will mean you have the contents of your discussion written down, plus the name of the HRT, or other product, you have decided to take.
You don’t have to have HRT
The doctor may think they know what’s right for you, however, they will accept that you have your ideas, concerns and expectations, and if you decide not to take HRT, after an effectively managed consultation, that’s perfectly fine.
It’s always easier for both parties if the patient has the disease, the doctor offers the treatment, and the patient takes the treatment and gets better. However, in real life this is not very often the case! The diagnosis may be uncertain, the patient may go home with the treatment – but not take it, and the condition may or may not get better on its own.
Time is a tool
Remember time is a tool. If you decide to take HRT today, you are not deciding to take it for ever. You can try it, say for 3 months and then reconsider. How has it made you feel? Are you better than you were 3 months ago? What have you liked what have you not liked?
How long before HRT starts to work?
In general, the benefits of HRT are seen soon after starting. Usually within 2 – 3 weeks, hot flushes will have abated; night sweats will be significantly reduced, and you will be sleeping better. However, increasing benefits are seen as treatment continues. Be patient, as it can take some months to find the best type, dose and formulation for you to get an optimal response. A 3-month check is still very early days.
No battle lines to be drawn
The menopause consultation should not be seen as one of conflict. If you’ve been suffering, you enter the arena already battle-weary from your menopausal symptoms! The healthcare professional you see will be on your side, not the enemy. They have no hidden agenda, just an empathetic wish to help you feel better.
The healthcare professional needs to offer a warm, empathetic and unhurried approach.
It’s not a case of them trying to force you to have HRT against your control. It’s a case of you exploring your options, which include HRT, non-hormonal treatments, and alternative therapies, considering the risks and benefits and them supporting you to make a decision about what is ultimately best for you.
The ‘Window of Opportunity’
The menopause is actually a wake-up call that none of us live forever, and old age beckons. So how can we live a healthy, disability-free old age? We can start my making good decisions about managing the menopause.
To get the best benefits from HRT, it should be started within 5 years of the onset of symptoms and taken for 5 to 10 years. For most women this will be around the age 50 to 60. This is called ‘the window of opportunity.’ Don’t miss yours!
By writing this article, I’m hoping you will take the initiative to go and have an effective consultation with your menopause specialist. Don’t miss out on the opportunity to make the best decisions about your medical care at and after menopause. Make sure your menopause is managed the best way it can be.
You may now know more than your doctor!
References
- Menopause Management – Getting Clinical Care Back on Track, by Manson J.E & Kaunitz A.M. New England Journal of Medicine (NEJM) 347:9 March 3rd, 2016
- Breast Cancer Facts & Figures 2017-2018 by Atlanta: American Cancer Society, Inc. 2017.
- Risks and Benefits of HRT before and after a Breast Cancer Diagnosis by the British Menopause Society, November 2018
- Decision making – Is it an Art or a Science by Colin G Smith, Awesome Mind Secrets , March 27th 2013
Information about Menopause and HRT
To find out the facts about the benefits and risks of HRT, take a look at these reliable sources of information –