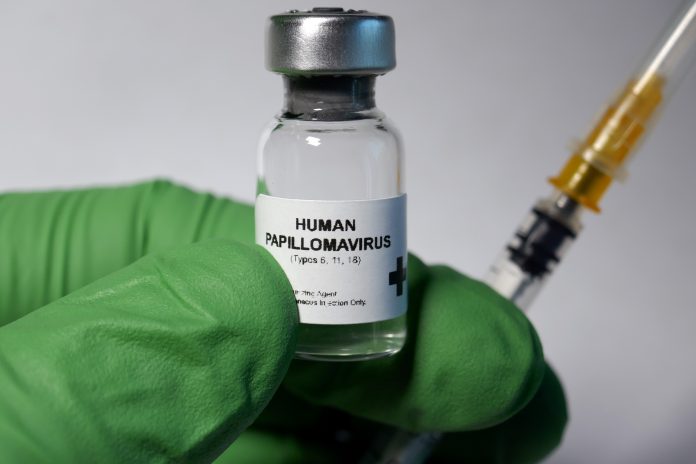
HPV is the most common STI in the world, affecting 80% of the population. Here, Dr Deborah Lee, from Dr Fox Online Pharmacy, addresses the most common issues about the condition
Discussing HPV with a patient in the sexual health clinic is one of the hardest conversations to have. At least with chlamydia, a patient may know how they got the infection, they can be given a successful antibiotic treatment, and afterwards, a test can be taken to show the infection has cleared.
With HPV – the reverse is true. The patient is often mystified as to where it came from, worried their partner has been unfaithful, full of anxiety about living with the infection in the future and being unable to have a test to show whether it is still present or has disappeared.
HPV affects 80% of the population
It’s important to try and normalise the situation – they have joined the ranks of the 80% of the population who have it. There’s every chance it will disappear by itself within 2 years. They must not feel ashamed or beat themselves up over it. If there is obvious distress the patient may need a referral for psychosexual counselling.
What is HPV?
HPV stands for human papillomavirus. HPV is the most common STI in the world. By the time we reach the age of 50, 80% of us have encountered the HPV virus, which is shed from the skin and from mucosal surfaces such as the mouth, the vagina, the urethra (the tube that runs down the centre of the penis), and the anal canal.
HPV is a DNA virus. It enters the body through tiny breaches in the skin and reproduces in the basal layers of the epithelium (skin). The virus is clever and often avoids immunological detection by the host, meaning it can persist for long periods, often months or years, and can be difficult to treat. This means the virus has become dormant, and it can stay in this state for 10 -20 years, only to reactivate in later life.
HPV statistics
3.2% of women are believed to have high-risk HPV in their cervix in the UK, at any one time.
Estimates suggest 8 in 10 people will be infected with HPV at some stage in their lifetime. But the vast majority will be completely unaware.
What are the types of HPV?
According to the National Library of Medicine, there are over 200 different subtypes of HPV.
- HPV 1,2, 4, 27 and 57 – cause warts on the skin and the soles of the feet (verrucas). These are a nuisance but do not have malignant potential.
- HPV 6 and 11 – low-risk oncogenic (cancer-causing) subtypes that most often cause anogenital warts.
- HPV 16 and 18 – the most common, high-risk oncogenic subtypes which cause cancerous or precancerous changes on the cervix (the neck of the womb), male and female anogenital regions, and the pharynx (mouth).
Most subtypes of HPV are asymptomatic
It’s extremely common for HPV to be present but for the person to be totally unaware of it, and have no symptoms or signs. At present, there are no agreed tests for HPV – apart from in research studies. People only know if they are HPV positive if they develop visible genital warts or have HPV detected with a cervical smear (see below).
HPV and its natural progression
9 out of 10 cases of HPV disappear by themselves eventually – usually after 12 months or so. The body mounts an antibody response which destroys the virus. But some people, for reasons that are unclear, can have persistent infection with high-risk HPV and hence remain at increased risk of cancer at the affected site – oropharynx (the mouth and throat), vulva, vaginal, penis, or anus.
What is the HPV vaccine?
Three HPV vaccines have been developed which are collectively effective against 9 different HPV subtypes.
Three HPV vaccines
- Gardasil (2006) – protective against HPV 6 and 11, and HPV 16 and 18.
- Cervarix (2007) – protective against HPV 16 and 18.
- Gardasil-9 (2014) – protective against HPV 6, 11, 16, 18, 31, 33, 45, 53 and 58.
Since 2012, Gardasil has been used to immunise school children between the ages of 12 and 13 (year 8). This is because girls and boys need to be vaccinated before they become sexually active.
What do we know about the safety of HPV vaccines?
The HPV vaccines are safe, with very few contraindications.
HPV vaccination is currently not recommended for women during pregnancy, although if a vaccine has been given inadvertently, current data does not show it causes harm to mother or baby. The vaccine can be given during breastfeeding. The most common side effects are redness and pain at the injection site, or headache, although most report no side effects at all.
The schedule for having the HIV vaccine involves having two injections, a first one and a second one, 6 to 24 months later. However, in June 2022, the vaccination used was switched over to Gardasil-9. Anyone up to age 25 is eligible to have Gardasil-9 free on the NHS. Up to age 45, the HPV vaccine can be purchased and administered privately.
How does the HIV vaccine work?
The HPV vaccine used proteins which act as virus-like particles (VLPs). These trick the body into thinking it has been in contact with the HPV virus, and hence antibodies are produced. In the future, if the HPV virus does enter the body, the immune system remembers it has seen this before and quickly produces antibodies which destroy the virus before it can become established.
What is the vaccine efficacy
The HPV vaccine is highly effective at preventing cervical cancer. HPV is believed to cause 99% of cases of cervical cancer. The HPV vaccination programme started in 2008. Over the following 11 years, rates of cervical cancer in those in their early 20’s, who were given the vaccine aged 12 or 13, dropped by 90%. Estimates suggest that during this time the HPV vaccine prevented 450 cases of cervical cancer, and 17,200 cases of precancerous changes on the cervix.
Other studies have shown that the HPV vaccination is effective in preventing HPV infection, genital warts and high-grade precancerous changes in the cervix.
Even though the vaccine is highly effective, women should still have regular cervical smears. The currently available vaccines do not protects against all HPV subtypes.
Understanding HPV transmission
HPV is transmitted by skin-to-skin contact or via skin-to-mucosal surfaces. This means it is spread by touching, and petting, and does not necessarily require sexual intercourse.
It is spread by all types of sexual activity/genital-to-genital contact – peno-vaginal, peno-oral and peno-anal sex. It is not spread in blood or semen. But it can be transmitted for example, on fingers, the outside of a condom, gloves, sex toys, and tubes of lubricant.
It is not spread in blood or semen.
HPV can live under the fingernails, meaning it’s possible to infect yourself!
This has been demonstrated in those who have never had sex and in children.
HPV is very infectious. Most people are unaware they are HPV positive. Hence it is most often passed on completely inadvertently. 70% of sexual partners of anyone who has an HPV infection are likely to become infected.
Babies can become infected after passage through an infected birth canal.
Babies can become infected after passage through an infected birth canal. This can cause polyps on their vocal cords – juvenile papillomatosis.
It is so common to be HPV-positive that we need to regard it as a normal part of life. It’s important to try not to be ashamed if you find you are HPV positive or develop warts. 80% of those aged 50 have been exposed to the HPV virus at some stage in their lives.
The best way to protect yourself from HPV is to have an HPV vaccination.
How can a woman in a long-term relationship get HPV?
Being married or in a long-term relationship does not prevent a woman from being infected with HPV. Many women erroneously think they cannot be at risk of HPV – but this is not the case. HPV is so common – every woman has to consider herself at risk. It also does not mean she or her partner has been unfaithful.
The virus can be present in the body for a long time – even years – before it is detected. The woman may well have been infected before she met her current partner – her husband. She could have even become infected the first time she had sex. The HPV virus can become dormant and rest inside the body for many years, even decades, before it becomes active.
Her husband may have infected her when they met, however long ago that was, but neither of them knew until now.
Sadly, women can get infected when receiving medical care. In one study 17.9% of gynaecological equipment tested positive for HPV, with contamination being nearly three times higher in private clinics than in hospital clinics. Infected sites included sterile gloves and colposcopy equipment.
contamination being nearly three times higher in private clinics than in hospital clinics
It’s important to be sensitive as she could also have been sexually assaulted in the past or raped.
The woman might work in a healthcare setting and have picked up HPV at work, on her fingers, by touching an infected piece of equipment and inadvertently passed it to the vulva or vagina, perhaps when wiping herself in the toilet.
It’s true that either she or her husband could have recently had – or have had – other sexual partners. But this may not be the case at all. If a woman does test positive for HPV, it’s important to reassure her that this does not mean her partner has been unfaithful.
What are the symptoms of HPV in women?
Most often, HPV does not cause any symptoms. The majority of women (and men) with HPV are unaware they have it.
However, HPV causes genital warts – which are small bumps, often rough to the touch, which can be darkly pigmented or flesh-coloured, and are found on the genitalia – the vulva, vagina, cervix, penis or anal skin. They may not cause symptoms or are sometimes itchy.
HPV is routinely tested for when a woman has a cervical smear. This may be the only way a woman knows she carries the virus. If this is high-risk HPV, and she has abnormal cells on the smear, she will be referred to the colposcopy clinic, where her cervix can be examined in greater detail and biopsies taken. If she is high-risk HPV positive but has a normal smear, she will simply be asked to have a repeat smear in 1 year’s time.
HPV also causes anogenital malignancies – vulval, vaginal, penile and anal cancers. The precursor to these cancers are precancerous changes in the skin called intraepithelial neoplasia – known respectively as vulval intraepithelial neoplasia (VIN), vaginal intraepithelial neoplasia (VaIN), penile intraepithelial neoplasia (PIN) and anal intraepithelial neoplasia (AIN).
These conditions present as small discoloured, raised or sometimes ulcerated, patches on the anogenital regions, which can be itchy and sometimes bleed. They can be flesh-coloured, red, pink or brown, and the skin is often thickened.
Although HPV is a causative factor, the herpes simplex virus, a weakened immune system, and smoking are also implicated.
When to seek medical help
If a woman notices any usual skin patches or changes in the genital region it’s vital to see her GP or go to the Sexual Health Clinic. The diagnosis is made on a biopsy. As with all medical conditions, getting a prompt diagnosis gives the best chance of a good outcome.
HPV testing is not routinely offered on the NHS. This is because the diagnosis can cause anxiety and distress and there is no current way to eradicate it from the body. HPV is tested for when cervical smears are taken. Women are not recommended to get tested for HPV under the age of 25.
Can HPV be cured?
There are no current treatments for HPV. Any lesions it causes, such as genital warts or changes to the cervix are treated, to get rid of the abnormality and help prompt the immune system to produce a better antibody response.
Don’t smoke – Smoking is a well-recognised risk factor for cervical cancer. Noxious chemicals in cigarette smoke impair the immune response to cervical HPV infection. Giving up smoking can lead to the resolution of abnormal cells on the cervix. Smoking allows the virus to grow and divide more rapidly. If a woman has an abnormal smear, stopping smoking will greatly improve her chances of recovery.
Genital warts are treated with a range of different options including cryotherapy, topical treatment such as podophyllin, or the use of Imiquimod (a cream which stimulates the antibody response). They can be surgically removed using electrocautery or laser.
How often do people infected with HPV develop cancer?
The majority of people infected with HPV will never know they are infected and will never develop cancer.
90% of women with HPV will become clear of the infection within 2 years of being infected.
In the 10% with ongoing infections, only a small percentage will go on to develop abnormal smears.
High-risk HPV is said to cause 3% of cancers in females, and 2% of cancers in males.
Overall, persistent HPV virus infection is thought to be responsible for 5% of cancers.
HPV in men
HPV affects men just as it does women. It causes genital warts on the penis and in the anus and around the anal margins. It can cause PIN and AIN, which can be low-grade or high-grade and can progress to penile or anal cancers.
How long can HPV be dormant?
No-one is quite sure of the answer to this question. HPV infection has a long latent phase which can last 10-20 years before the development of cervical cancer occurs. After this time, if HPV is detected it’s hard to say if this is the same infection or a new infection with a different subtype.
Final thoughts on HPV
It’s a sobering thought that most of us will become infected with HPV during our lifetime. What we can do is ensure our young people are protected b making sure they are vaccinated before the become sexually active.
Meanwhile the burden of HPV exists, and we all have to live with it. There should be no shame or stigma attached to a diagnosis of HPV. Even those who have never had sexual intercourse can have HPV. We have to learn to live with HPV, like we have to accept other common infections like Covid-19.
For more information
- NHS – HPV
- paho.org – Frequently asked questions on HPV