The National Institute of Mental Health (NIMH) is the lead U.S. federal agency for research on mental illnesses
The mission of NIMH is to transform the understanding and treatment of mental illnesses through basic and clinical research, paving the way for prevention, recovery and cure – including research into perinatal depression.
To carry out its mission, NIMH conducts and supports biomedical and behavioural research, health services research, research training and health information dissemination with respect to the causes, diagnosis, treatment, management and prevention of mental illnesses.
As mental health is an important part of overall health, NIMH invests in research on adaptive and maladaptive behaviours to better understand mental function and dysfunction.
The NIMH Strategic Plan sets four goals to form a broad roadmap for the institute’s research priorities, spanning fundamental science to public health impact.
- Goal 1: Define the Brain Mechanisms Underlying Complex Behaviours.
- Goal 2: Examine Mental Illness Trajectories Across the Lifespan.
- Goal 3: Strive for Prevention and Cures.
- Goal 4: Strengthen the Public Health Impact of NIMH-Supported Research.
An introduction to perinatal depression
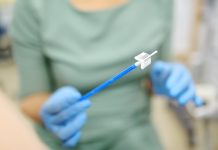
Perinatal depression is a mood disorder that can affect women during pregnancy and after childbirth. Perinatal depression includes depression that begins during pregnancy (called prenatal depression) and depression that begins after the baby is born (called postpartum depression). Mothers with perinatal depression experience feelings of extreme sadness, anxiety and fatigue that may make it difficult for them to carry out daily tasks, including caring for themselves or others.
Perinatal depression is a real medical illness and can affect any mother – regardless of age, race, income, culture or education. Women are not to blame or at fault for having perinatal depression: it is not brought on by anything a mother has or has not done. Perinatal depression does not have a single cause. Research suggests that perinatal depression is caused by a combination of genetic and environmental factors. Life stress (for example, demands at work or experiences of past trauma), the physical and emotional demands of childbearing and caring for a new baby, and changes in hormones that occur during and after pregnancy can contribute to the development of perinatal depression. In addition, women are at greater risk for developing perinatal depression if they have a personal or family history of depression or bipolar disorder or if they have experienced perinatal depression with a previous pregnancy.
Some women may experience a few symptoms of perinatal depression; others may experience several symptoms. Some of the more common symptoms of perinatal depression include:
- Persistent sad, anxious or “empty” mood.
- Irritability.
- Feelings of guilt, worthlessness, hopelessness or helplessness.
- Loss of interest or pleasure in hobbies and activities.
- Fatigue or abnormal decrease in energy.
- Feeling restless or having trouble sitting still.
- Difficulty concentrating, remembering or making decisions.
- Difficulty sleeping (even when the baby is sleeping), awakening early in the morning or oversleeping.
- Abnormal appetite, weight changes or both.
- Aches or pains, headaches, cramps or digestive problems that do not have a clear physical cause or do not ease even with treatment.
- Trouble bonding or forming an emotional attachment with the new baby.
- Persistent doubts about the ability to care for the new baby.
- Thoughts about death, suicide or harming oneself or the baby.
Only a healthcare provider can help a woman determine whether the symptoms she is feeling are due to perinatal depression or something else. It is important for women who experience any of these symptoms to see a healthcare provider.
Treatment for perinatal depression for both mothers and babies
Treatment for perinatal depression is important for the health of both the mother and the baby, as perinatal depression can have serious health effects on both. With proper treatment, most women feel better and their symptoms improve.

Psychotherapy
Several types of psychotherapy (sometimes called “talk therapy” or “counselling”) can help women with perinatal depression. Two examples of evidence-based approaches that have been used to treat perinatal depression include cognitive behavioural therapy and interpersonal therapy.
Cognitive Behavioural Therapy (CBT)
CBT is a type of psychotherapy that can help people with depression and anxiety. It teaches people different ways of thinking, behaving, and reacting to situations. People learn to challenge and change unhelpful patterns of thinking and behaviour as a way of improving their depressive and anxious feelings and emotions. CBT can be conducted individually or with a group of people who have similar concerns.
Interpersonal Therapy (IPT)
IPT is an evidence-based therapy that has been used to treat depression, including perinatal depression. It is based on the idea that interpersonal and life events impact mood and vice versa. The goal of IPT is to help people to improve their communication skills within relationships, to develop social support networks and to develop realistic expectations that allow them to deal with crises or other issues that may be contributing to their depression.
Medication
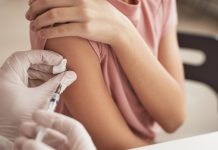
Women with perinatal depression are most commonly treated with antidepressants, which are medications used to treat depression. They may help improve the way the brain uses certain chemicals that control mood or stress.
Researchers at NIMH and around the country conduct many clinical research studies with patients and healthy volunteers to continue the development of treatments for perinatal depression.