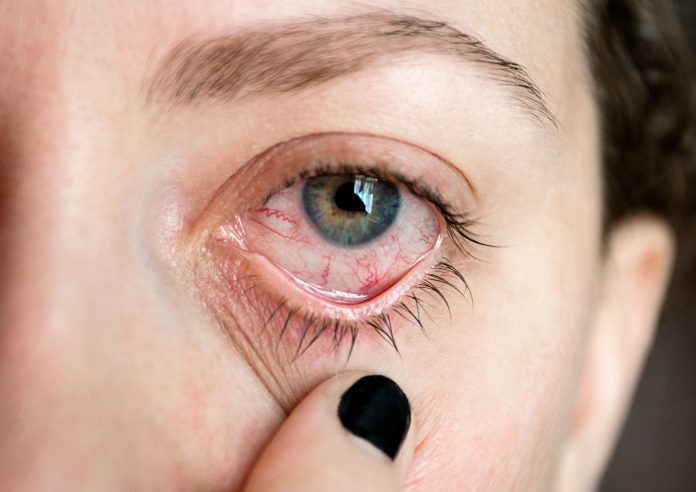
Dr Gerry Morrow explains what you need to know about an aspect of ophthalmology called uveitis, defined as inflammation of the uveal tract, which comprises the iris, ciliary body and choroid
How easy is it to diagnose sub-types of uveitis?
Uveitis is defined as inflammation of the uveal tract, which comprises the iris, ciliary body and choroid. Inflammation may be more generalised to include the retina, the optic nerve, and the vitreous humour, known as panuveitis. (1)
This inflammation can be acute, recurrent or chronic. The most commonly affected age group is between 20-60, but it can also affect children. There are a multiplicity of causes of uveitis, including autoimmune disorders, cytomegalovirus and other infections. (1)
Symptoms and signs can be insidious and subtle, they include redness of the eye, pain, photophobia, a watering eye and sometimes (but not always) reduced vision associated with sluggish pupillary reactions.
The diagnostic problem for clinicians is three-fold:
1. There is a very long list of differential diagnoses, including relatively innocent causes of red-eye, including simple and common viral conjunctivitis.
2. A slit lamp examination is required (and the associated expertise) to make a substantive diagnosis.
3. This is a relatively rare condition; a GP may see fewer than one person a year with a new diagnosis of uveitis.
Early diagnosis is crucial to prevent the possible complication of visual loss due to secondary macular oedema, cataract and glaucoma. (2)
Given all of these problems how easy is it to make a definitive subtype diagnosis of this important and problematic condition?
According to a paper in the American Journal of Ophthalmology, the answer is ‘not very easy.’ The authors set out to measure how likely uveitis experts were to agree on a diagnosis of sub-types of uveitis in 5766 patients. 76 investigators and nine committees reviewed case notes and images for all these patients and reported on how much agreement on a specific diagnosis there was between reviewers. (3)
Their analysis relied on the concept of measuring interrater reliability, which is the correlation statistic kappa (k). If k = 1 this means that both clinicians agree exactly on a diagnosis. If k = minus 1 then there is complete disagreement. Most research is based on figures of k= 0.81 to 1 as providing ‘almost perfect’ agreement. (4)
In the uveitis interobserver agreement paper, it was found that even amongst uveitis experts’ variability was only ‘moderate at best’ as the whole series of 5766 patients, k = 0.39, with a range of 0.23-0.79. It was only when teleconferences were organised to create a consensus between clinicians that the variability correlation was moved much closer to complete agreement. (3)
Crucially this agreement has fed into a final dataset for machine learning in order to assist the development of clearer diagnostic criteria for each diagnostic class of uveitis.
It is hoped that this work will help GPs and other clinicians in their diagnostic challenge of managing patients with visual symptoms in order to exclude or refer people with possible uveitis.
References
1. NICE Clinical Knowledge Summaries Uveitis. Available from: https://cks.nice.org.uk/uveitis
2. The College of Optometrists Uveitis Clinical Management Guidelines. Available from: https://www.college-optometrists.org/guidance/clinical-management-guidelines/uveitis-anterior-acute-and-recurrent-.html
3. Jabs D.A. et al 2018 Interobserver Agreement Among Uveitis Experts on Uveitic Diagnoses: The Standardization of Uveitis Nomenclature Experience. American Journal of Ophthalmology Volume 186, Available from: https://www.sciencedirect.com/science/article/pii/S0002939417304592
4. McHugh M. L. 2012. Interrater reliability: the kappa statistic. Biochemia Medica, 22(3), 276–282. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3900052/
Dr Gerry Morrow
Medical Director
Clarity Informatics
Tel: +44 (0)845 113 1000
www.clarity.co.uk
www.linkedin.com/in/gerrymorrow
www.twitter.com/Clarity_hi
www.twitter.com/Clarity_Gerry