Scientists have created an ‘artificial pancreas’ that uses an algorithm to protect the body – especially ground-breaking for young children with type 1 diabetes
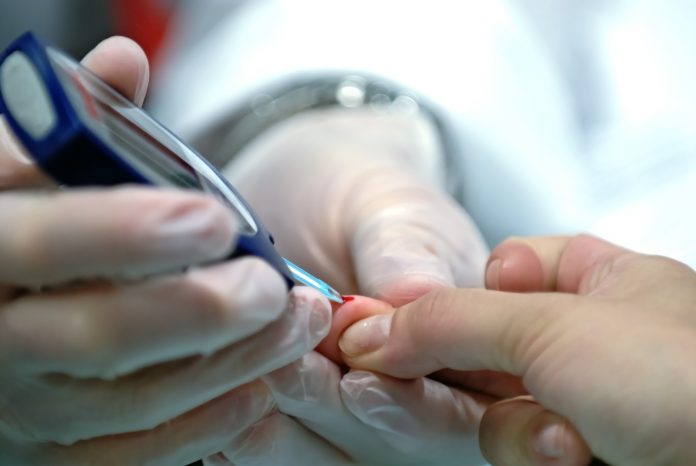
Type 1 diabetes is demanding, but especially so for very young children. Parents and caregivers face a dilemma – with children of that age being highly whimsical about their food intake and activity levels, creating immense risk of low blood sugar.
In August, 2021, scientists at Cambridge announced that their ‘artificial pancreas’ was working. A trial found that the pancreas, a mixture of algorithm and physical technology, significantly helped people with type 2 diabetes and kidney failure. This is great news, as the device can theoretically replace the intricate dance of insulin and finger-prick tests that face diabetes patients across the world.
Scientists in Sweden are also working on a potential ‘diabetes vaccine’ – but it remains very much a work in progress. Diabetes, being a comorbidity for severe COVID, is also highly prevalent in socio-economically deprived and BAME communities. Some experts have even proposed a more nuanced medical understanding of race, which would shape treatment targets to be more effective.
At the time of the first trial, Professor Roman Hovorka said the faux-pancreas “gave the users peace of mind.”
Now, the same device appears to be successful at managing the more labour-intensive type 1 diabetes in a crucial demographic – young children.
Dangerously low blood sugar levels, known as hypoglycaemia, and overly high blood sugar levels, known as hyperglycaemia, are the unforgiving borders of the safe window. If blood sugar changes dangerously, a young child is unable to vocalise that they are experiencing those symptoms.
This lack of clarity means that parents have to monitor blood sugar levels very closely. In the past, studies have linked hyperglycaemia in children with type 1 to slower brain growth.
So, how does the ‘artificial pancreas’ work?
An app, designed by Professor Roman Hovorka from the Wellcome-MRC Institute of Metabolic Science at the University of Cambridge, combined with a glucose monitor and insulin pump is the artificial pancreas. Working together, the app and technology deliver insulin based on real-time or predicted glucose levels.
At mealtimes, the carer will need to manually deliver insulin. But otherwise, the algorithm is capable of functioning with no human assistance. Right now, it isn’t available to buy.
Professor Hovorka, discussing the app, said: “CamAPS FX makes predictions about what it thinks is likely to happen next based on past experience. It learns how much insulin the child needs per day and how this changes at different times of the day. It then uses this to adjust insulin levels to help achieve ideal blood sugar levels.”
74 children, aged between one to seven
For 16 weeks, across seven places in the UK and Europe, a team examined how the hybrid closed-loop therapy with sensor-augmented pump therapy really worked.
They compared the artificial pancreas to a control treatment, which was just an insulin pump attached to a sensor.
The children, on average, spent 71.6% of their day in the target range for glucose levels when using the artificial pancreas via the CamAPS FX app. This is almost nine percentage points higher than the 16 weeks they spent on just the sensor-augmented pump.
That is essentially an extra 125 minutes per day in the target range.
The children also had less than a quarter of their time, 22.9%, with raised blood sugar levels while using the app. In the alternate therapy, these same children were in hyperglycaemia for nine more percentage points.
There was no difference in the time spent in hypoglycaemia.
The tech solves the ‘night-time problem’
One of the biggest challenges reported by families of young children with type 1 diabetes is poor sleep quality, as variability in insulin requirements and parental fear of hypoglycaemia are highest overnight. In their study, the researchers found that more than 80% of overnight sensor readings were within the target range, showing that hybrid closed-loop therapy addresses the ‘night-time problem’ more effectively than sensor-augmented pump therapy.
When it comes to night-time, parents experience the terror of not knowing if their child will have secure blood sugar through those dark hours. This fear leads to poor sleep quality, as childhood differences in activity and food mean that insulin times change – constantly. This change means parental fears of hypoglycaemia are highest overnight.
This study found that 80% of overnight readings were within the target range, putting parental fears at ease.
When can parents get this device for their children?
So far, it is available through selected NHS trusts. The team hope to push for even more devices to become accessible through the NHS, soon.
Professor Hovorka further said: “From the first clinical trials of our algorithms to today’s findings has taken well over a decade, but the dedication of my team and the support of all the children and families who have taken part in our studies, has paid off. We believe our artificial pancreas will transform the lives of families with very young children affected by type 1 diabetes.”