Cancer Centre London’s Keisha Robinson spoke to Open Access Government about cancer treatment in the UK today, in particular, radiotherapy
Cancer Research UK believes it’s crucial to fund doctors, nurses and scientists to help beat cancer sooner rather than later.(1) Research in the field concerning the prevention, diagnosis and treatment of cancer has saved millions of lives.(2) Today, radiotherapy is one of the main treatments for cancer after its pioneering use during the 1920s and 1930s. Millions globally benefit from radiotherapy annually and the treatment cures more individuals than cancer drugs do, in the view of Cancer Research UK.(3)
In this interview, Keisha Robinson, Head of Radiotherapy and Quality at the Cancer Centre London explains how radiotherapy works to treat cancer. We find out if whether you have radiotherapy as part of your treatment depends on what type of cancer you have. Keisha unpacks what we need to know about palliative radiotherapy and finally, where she sees the field heading in the future, including research priorities.
What is radiotherapy? How does radiotherapy work to treat cancer?
Radiotherapy is the use of high-energy particles or waves, such as x-rays, gamma rays or protons to destroy or damage cancer cells. Treatment is safe and effective.
Sometimes radiation therapy is the only treatment a patient needs. At other times, it is only one part of a patient’s treatment pathway. For example, prostate cancer is often treated with radiotherapy alone, while breast cancer patients may be treated with surgery, chemotherapy and radiotherapy.
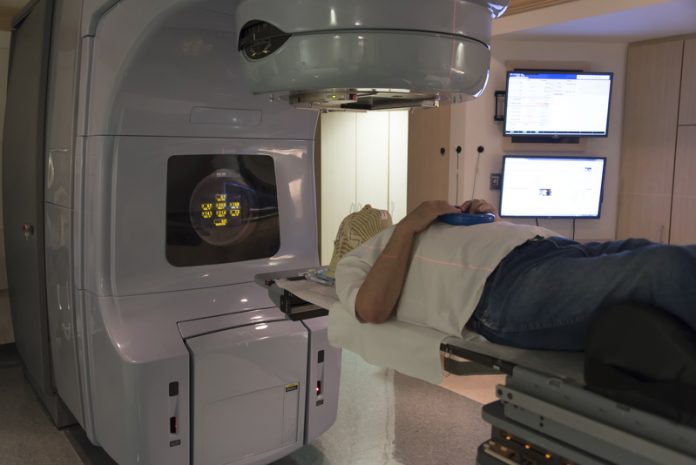
Radiotherapy can be given in three ways: external, internal or systemic radiation. External radiation uses a machine that directs high-energy X-rays from outside the body into the tumour. Internal radiation (brachytherapy) involves putting a radioactive source inside the body or near the tumour, and systemic radiation refers to radioactive drugs given by mouth or put into a vein. These drugs then travel throughout the body.
Does whether you have radiotherapy as part of your treatment depend on what type of cancer you have?
The type of radiotherapy you get will depend on the type of cancer and where it is. Computerised personalised treatment plans and specialised quality assurance safety checks are undertaken before any treatment is started.
External radiation treatment takes only a few minutes, usually given over a number of days or weeks as an outpatient. This means that many patients can continue their normal routines, but some people may develop side effects, that are related to the region of the body treated.
Tell us also about palliative radiotherapy – radiotherapy to control and relieve symptoms and improve quality of life and side effects
Palliative radiotherapy aims to shrink cancer, slow down its growth or control symptoms. It doesn’t aim to cure cancer.
Patients might have palliative radiotherapy to:
• Relieve bone pain.
• Treat pressure on the spinal cord (spinal cord compression).
• Shrink a tumour to relieve pressure or a blockage.
• Treat symptoms of cancer in the brain.
• Treat symptoms of cancer in the lungs.
• Control ulcerating cancer and reduce bleeding.
• Treat a blood vessel blockage in the chest called superior vena cava obstruction (SVCO).
The treatment is planned using information from a planning CT scan.
The radiotherapy is given from outside the body using an Elekta Versa HD linear accelerator and image guidance is used to deliver highly accurate treatment. The treatment is completely painless, delivered in about 10 minutes, and is given with the patient in a comfortable position on the treatment couch. The number of treatment fractions varies from a single treatment fraction to 10 fractions.
One approach is the ‘see, plan, treat’ treatment pathway for patients requiring palliative radiotherapy. This means the patient will be seen by a consultant, have their planning session and then treatment delivery on the same day. This pathway is particularly beneficial for patients as it avoids multiple visits.
Where do you see the field of radiotherapy heading in the future and what are the priorities for research in the field?
Technology is continuing to evolve at some pace, and it is making a huge impact on patient care. Some of the latest technology includes highly sophisticated radiation treatment delivery machines that can enable high-precision treatment in managing a range of cancers, including those in the head and neck, lung, breast and prostate. These machines are used to deliver advanced, highly targeted stereotactic external radiation treatment to the brain, lung, liver and bones.
Other advances improve the accuracy and safety of radiation delivery, such as heart-sparing radiation treatment for left-sided breast cancer, using the Active Breathing Coordinator (ABC) system.
Some of the latest advances in technology have improved patient outcomes. For example, some cancer centres can offer relatively new ‘tattooless’ radiotherapy using new high-tech 3D camera technology – ‘AlignRT®’. This means patients no longer need to receive permanent markings before starting radiotherapy treatment. In addition, this camera technology can monitor the position and movement of patients in ‘real-time’, further enhancing the safety and accuracy of radiation treatment.
References
1 https://www.cancerresearchuk.org/about-us
2 https://www.cancerresearchuk.org/our-research
3 https://www.cancerresearchuk.org/our-research-by-cancer-topic/our-research-into-radiotherapy