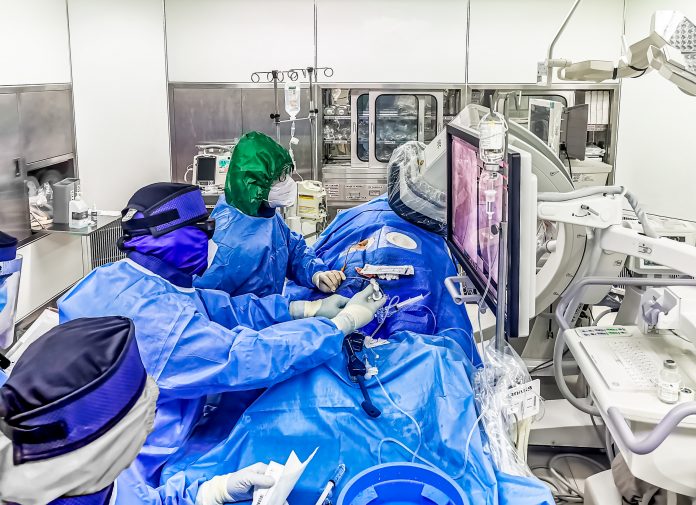
Dr Timothy Fairbairn, Consultant Cardiologist at Liverpool Heart & Chest Hospital and Dr Campbell Rogers, Chief Medical Officer at HeartFlow, discuss how cardiologists are responding to the ongoing COVID-19 pandemic and why digital innovation is crucial
There has been a remarkable growth of digital technologies making waves in the health space in recent years. The HeartFlow Analysis is one of these. Available in over 50 NHS England hospitals, the non-invasive technology takes data from a coronary CT, uses deep learning (a form of artificial intelligence) and a team of highly trained analysts to create a digital, 3D model of a patient’s arteries. The technology then solves millions of complex equations to provide a measurement of blood flow in the coronary arteries, identifying areas where flow may be compromised.
In this interview with both Dr Timothy Fairbairn, Consultant Cardiologist at Liverpool Heart & Chest Hospital and Dr Campbell Rogers, Chief Medical Officer at HeartFlow, they explain more about the technology, how cardiologists are responding to the ongoing Covid-19 pandemic and why digital innovation is crucial to the future of patient care within the health service.
What is the HeartFlow Analysis and how is it being used within the NHS?
Dr Fairbairn: Heart care has evolved significantly in recent years. In the past, a patient who had chest pain and possible coronary heart disease (CHD) would be investigated with stress tests or invasive tests. Leveraging NICE’s recommendations, the NHS has now embraced a CT-first approach. This is less invasive, less risky but still a highly sensitive test. This approach allows clinicians to look at the coronary arteries and identify patients who can be managed medically or require further assessment, potentially with the HeartFlow Analysis.
The HeartFlow technology helps doctors to find out if any narrowings are impacting blood flow in a patient’s arteries, which allows them to determine the best treatment plan. This improves the diagnosis and management of coronary heart disease (CHD), the UK’s biggest killer.
I was lucky to be an early adopter of the technology, and have seen its ability to improve patient care. It allows us to get the right patient to the catheterisation lab so that they can get the right treatment as quickly as possible. In our practice, we’ve found that four out of five patients who have a HeartFlow Analysis avoid the need for further invasive testing.
Have you seen a change in how doctors are managing cardiovascular disease during the Covid-19 pandemic?
Dr Fairbairn: Covid-19 has placed many challenges on us as doctors and as patients. The disease has various cardiovascular complications which we need to help manage, but a major concern has been the impact on people who don’t have coronavirus. As cardiologists, our primary concern is being able to identify and treat patients who have a severe risk of future heart attack and other CHD-related complications. We have seen that many patients are not coming to the hospital despite symptoms of CHD, including chest pains, which can occasionally result in potentially fatal heart attacks. We need to reassure patients that it is safe to come into the hospital for their assessments and treatments so that more lives are not lost as an indirect consequence of the pandemic.
Many patients with heart problems are considered ‘high risk’ when it comes to contracting Covid-19, so we have to very carefully balance the risk of bringing them into hospitals or allowing them to stay at home. Our management of CHD hasn’t changed significantly in light of the pandemic, but the way we’re triaging patients has.
Where we can, we’ve begun seeing patients virtually, to understand more about their symptoms and to help us calculate any risks. When we think it’s essential that our patients come in for further investigations, we are taking every precaution and using PPE throughout any investigative procedures. We also take into consideration things like the time it takes to run a certain type of diagnostic test and the proximity required between medical professionals and patients during such testing. As such, the pandemic has reinforced coronary CT as an ideal test, allowing us to rapidly rule in or rule out the presence of CHD with minimal exposure.
At Liverpool Heart and Chest, we’re fortunate to have two cardiac CT scanners available which means that one can be used in monitoring patients with Covid-19, while the other can be used for broader cardiac investigations.
Being able to use the HeartFlow Analysis means we’re able to accurately diagnosis CHD with a single patient visit. If we determine that we need more information to make a definitive diagnosis, we can directly send images from the CT scans to HeartFlow, requiring no additional patient time in the hospital or exposure of our staff to patients. Anatomical information from a CT scan and functional information from HeartFlow can help us determine which patients can be treated with medication alone, which means that we don’t need to bring them back to the hospital.
How do you stratify risk and decide which patients you need to prioritise?
Dr Fairbairn: An initial virtual conversation with our patients can help us establish the groundwork on their risk factors. It’s important for us to understand what symptoms they’re experiencing and if the symptoms are getting more severe. We can also take into account wider lifestyle and genetic factors that could contribute to a diagnosis of CHD.
My colleagues and I have now put in place tiering systems to help stratify risk within our patients. This helps us identify patients who are at highest risk of CHD and need to undergo a diagnostic test. By encouraging everyone along the patient care pathway to think in these terms, we’re aiming to make sure that urgent care is still delivered to those who need it most, while making sure our staff are fully protected too.
After the pandemic is over, what do you expect will happen to patients with symptoms of heart disease?
Dr Rogers: This is an interesting question, as we do need to be mindful that some patients may be remaining at home during this pandemic due to fears of contracting the virus. On top of this, it could be the case that some trusts have had to extend the waiting times for evaluation of some patients with suspected CHD because they have had to prioritise those with coronavirus.
Digital technologies are going to be and will remain key to managing patients in a way that helps to improve patient care and prioritise those that are most in need of treatment.
The use of CT and HeartFlow will aid in identifying and reducing wait times for those patients who need to go to the catheterisation lab.
Even before the pandemic, evidence across a number of sites using the HeartFlow Analysis found it was greatly reducing wait times and helping hospitals to deliver definitive CHD diagnoses to patients quickly.
Finally, how do you see the health service using digital technologies after the pandemic?
Dr Rogers: The coronavirus pandemic has created unique challenges for many healthcare systems around the world and the NHS has not been immune. The pandemic has demonstrated the importance of digital technologies, particularly when it comes to triaging patients and using hospital time and resources more effectively.
When elective services resume, technology and the data it unlocks are likely to become increasingly important to clinicians seeking to offer the best patient care while juggling high demand.
This may open the door to greater uptake of digital innovations across the health service. In the meantime, tried and tested technologies such as HeartFlow will continue to play a significant role in delivering an accurate, streamlined approach to cardiac care, prioritising further treatment and testing for those who need it most.