Justin Hall, GM and VP EMEA, iRhythm Technologies, explores how modern technology is helping to diagnose Atrial Fibrillation (AF)
This time last year there was no way of predicting what we were about to face – one of the toughest health emergencies in history. Whilst our National Health Service – which was already severely under-resourced and oversubscribed – has been stretched to breaking point during this time, it has adapted admirably in order to ensure that the general public are still able to access the treatment and advice that they need.
In fact, the entire healthcare industry has witnessed significant shifts to the delivery of patient care. In order to continue to deliver regular services, whilst managing the influx of COVID-19 cases, GPs, nurses, manufacturers and many other healthcare professionals have had to adapt and embrace new models and practices.
One area that has been forced to drastically remodel its patient delivery is the diagnosis of serious conditions, especially those related to the heart. When dealing with cardiac issues, every second counts. Whether in the midst of a global pandemic or not, getting an accurate diagnosis as quickly as possible could be the difference between life and death.
Making diagnosis a priority
With concerns around the ongoing pandemic becoming a primary talking point this year, cardiac health has taken a backseat for many individuals. After all, quite often when it comes to heart conditions there are no warning signs and the patient can remain symptomless until a more serious event occurs, such as a stroke or heart attack.
In recent months many individuals have, understandably, cancelled appointments or delayed seeking medical advice if unrelated to COVID-19. Whether in an effort to limit their own exposure to the virus, or avoid putting additional strain on an already stretched healthcare system, the latest NHS Digital statistics estimate that there have been around 26 million fewer GP visits during this time.
Add to this the number of routine cardiac treatments that have been delayed in order for resources to be used elsewhere, and it’s clear that the pandemic will continue to indirectly impact cardiac care for several years. There’s just no way of knowing how many underlying conditions will have gone undiagnosed during this time period, and the potential backlog that that could create for medical staff moving forward.
Although navigating the current health crisis is the primary focus at the moment – as it should be – we still need to ensure that individuals suffering with other conditions are able to access the diagnostic tools and medical advice that they need. This is why many providers of diagnostic technologies have changed the way that they deliver their services, in order to ensure that patients can still access them, even when they need to stay at home and isolate.
Delivering remote care for the most serious conditions
In order to keep all parties safe, while also reducing some of the strain being placed on healthcare resources, some health tech providers have launched direct-to-patient shipping models.
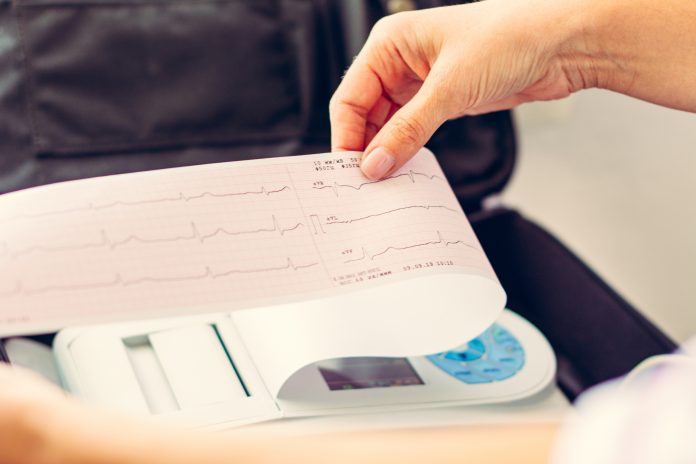
These models enable patients to access the latest in life-saving diagnostic tools, including self-application cardiac devices which are both patient-friendly and able to deliver on accuracy, even during a global pandemic. By providing uninterrupted, comprehensive monitoring and ECG interpretation for up to 14 days, these technologies ensure that there are no critical knowledge gaps from poor signal quality or data interruptions. They provide a clear and detailed look into a patient’s heart rhythm.
Not only does this streamlined service reduce the need for repeat testing – which results in greater pressure on the NHS and increased risk of exposure – it can also accelerate time-to-treatment for patients. This means that they get the help they need in a much shorter timeframe, potentially reducing their risk of suffering when linked to heart conditions, such as Atrial Fibrillation (AF).
AF is currently the leading independent risk factor of stroke, contributing to one in five across the UK alone. But that’s not all. AF also increases the severity of a stroke, with research discovering that those suffering are twice as likely to die, and three times more likely to become disabled as a result.
Many sufferers won’t even know they have AF until they actually experience a stroke. In fact, it’s thought that up to a third of those currently living with the condition remain undiagnosed. This number is only likely to have increased during the pandemic, as many opportunities to diagnose the condition effectively will have been missed.
This is where direct-to-patient shipping models come in. As with many heart conditions, the key to improving the outcome of AF – and therefore the associated risk of stroke – is through earlier and more accurate detection. Through these models, an individual can be diagnosed sooner, meaning medical practitioners can deploy the best course of treatment in a much more timely manner.
Getting one step ahead
Throughout this year of challenges, our healthcare industry has adapted in order to ensure that each and every one of us can continue to access the treatment we need. With the first COVID-19 vaccinations being administered in the UK this month, there is hope that we can start to move forward. However, the backlog of missed appointments and resulting missed diagnosis is impossible to ignore.
As we begin the new year, the remote models and services that we have adopted will prove to be more important than ever, especially when it comes to diagnosing and treating the most serious cardiac conditions. The diagnosis landscape has changed forever and we must be sure to carry forward the lessons learned and successes we have experienced in recent months. It is only then that we can ensure that our healthcare system is sustainable long-term.







I currently am wearing a ZioXT monitor..looking through the website to become more informed…thank you!