The University of Manchester finds that Flash technology is better than finger-prick testing, keeping diabetes patients at a good blood sugar level – for an extra two hours per day
The accuracy of blood sugar level testing is directly linked with good management of the disease, which can then change a person’s survival chances if they should contract COVID. In 2021, Cambridge unveiled their “artificial pancreas”, which uses AI to help track blood sugar levels in type 2 diabetes patients. So far, it also remains in the testing stage – but could make the difference between life and death for individuals who live with either type of diabetes.
In this era of viral pandemic, type 1 diabetes is also a significant comorbidity for severe cases of COVID – as it is for a range of other illnesses.
“I think these data support prioritizing individuals with type 1 or individuals with type 2 diabetes for immunization alongside other high-risk medical conditions that increase the risk of getting very sick with COVID-19, such as heart or lung disease,” said Dr Justin Gregory, who was involved in a separate study examining the tripled risk of severe COVID in those living with diabetes.
What is a flash glucose monitoring system?
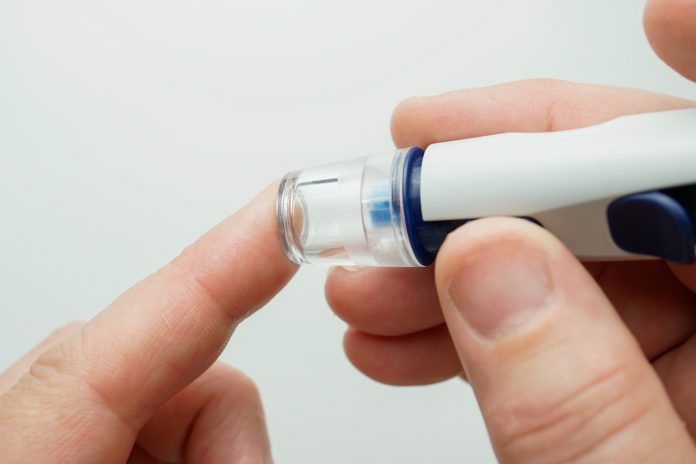
A Flash monitoring (FreeStyle Libre), is something that measures the amount of sugar in the fluid under the skin, throughout the day. Flash tech can help you to see sugar levels going up or down, how sugar levels change over time, and a view of the last eight hours, so medical experts or the patient can see what happened when they sleep overnight.
However, Flash tech looks at interstitial fluid, as opposed to actual blood sugar levels under the skin. Since they’re a few minutes behind blood sugar levels, finger-prick testing is still necessary from time to time.
Diabetes patients spent extra two hours in good blood sugar place
A University of Manchester team led by Dr Lalantha Leelarathna, conducted a clinical trial to learn if second-generation Flash tech is better and more cost-effective than traditional finger-prick testing for type 1 diabetes patients. The study was funded by Diabetes UK.
The clinical trial has 156 participants, with type 1 diabetes patients who had slightly too high blood glucose levels. For 24 weeks, half of the participants monitored their blood glucose with Flash and the other half continued using finger prick testing.
After 24 weeks, those participants who used Flash had reduced their HbA1c from an average of 71.6 mmol/mol to 62.7 mmol/mol – a reduction of 8.49 mmol/mol. Lowering HbA1c by this amount can decrease the risk of developing diabetes complications in the future by up to 40%.
In comparison, those in the finger prick group had reduced their HbA1c on average by only 2.2 mmol/mol by the end of the study.
The team found that those using Flash tech spent an extra two hours per day in the range of good blood sugar levels, 80% less time in the dangerously low range.
NHS spends 10% on diabetes, could be reduced via innovation
Dr Elizabeth Robertson, Director of Research at Diabetes UK, which funded the study, said:
“We want as many people as possible to have access to innovative diabetes technologies. This study confirms the radical improvements Flash can bring to the lives of people living with type 1 diabetes, helping them to reduce their blood glucose levels – protecting against short and long-term diabetes complications – and removing some of the relentless burden of managing the condition.”
“By demonstrating the benefits to people living with type 1 diabetes and the value for money to the NHS – which currently spends 10% of its budget on diabetes care – we hope these results encourage healthcare professionals and people with type 1 diabetes to consider flash glucose monitoring as a cost-effective and life-improving intervention.”
Flash tech could be life changing technology for type 1 diabetes
Dr Lalantha Leelarathna, Diabetes UK-funded researcher at University of Manchester, said: “Ability to monitor glucose without painful finger-sticks is life-changing for many people living with type 1 diabetes. With the use of second-generation Flash technology, we found significant improvements in average glucose levels and a reduction in both high and low glucose levels, helping people to spend more time with normal glucose levels thereby reducing their risk of long-term diabetes related complications.
“This intervention was highly cost-effective and led to high level of treatment satisfaction. We call for universal funding of this life changing technology for all people living with type 1 diabetes.”






Interesting reading on the Flash Tech. Is it available on prescription and can we now ask our doctors for it to be used now. If not when can type 1 patients start it.