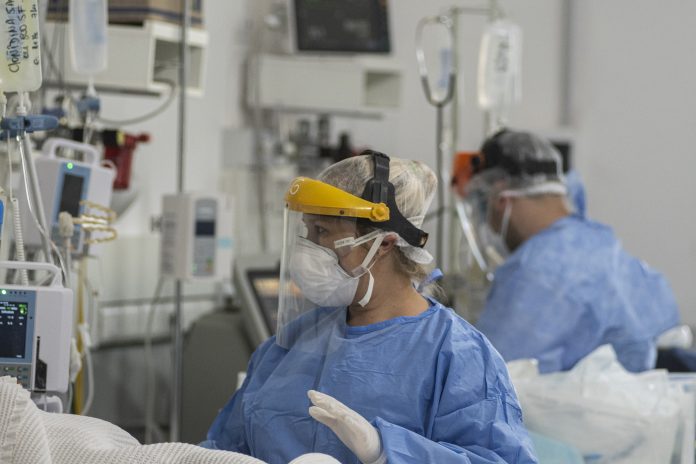
An international study examined hospitalised COVID patients across 11 countries – finding that obese patients are 73% more likely to need invasive respiratory support
The team worked across 11 countries, analysing whether weight was definitely a reason why some patients needed more severe COVID treatment than others. The Murdoch Children’s Research Institute (MCRI) and The University of Queensland found that overweight or obese patients have a more risky COVID outcome – with a higher likelihood of oxygen and invasive ventilation, than individuals with a healthy weight.
While obesity has been noted as a risk factor for worse COVID outcomes in the UK, this is one of the first cohesive investigations into just how weight can shape a person’s fight for survival when they are hospitalised with the virus.
What did the investigation find out?
The team reveal that COVID patients with obesity are more likely to need oxygen, with a 73% increased chance of needing invasive ventilation. Among 7244 patients, 34.8% were overweight and 30.8% were obese.
For COVID patients with diabetes, there was also an increased risk of invasive ventilation – but obesity plus diabetes did not increase that risk.
The evidence is ‘conclusive’
The University of Queensland’s Dr Kirsty Short, co-lead on the study, explained: “Obesity is associated with numerous poor health outcomes, including increased risk of cardiometabolic and respiratory disease and more severe viral disease including influenza, dengue and SARS-CoV-1.
“Given the large scale of this study we have conclusively shown that being overweight or obese are independent risk factors for worse outcomes in adults hospitalised with COVID-19.”
Address socio-economic reasons for obesity, says researcher
Almost 40% of the global population are overweight or obese.
Dr Danielle Longmore, MCRI researcher, suggested that new strategies to treat the complex socio-economic drivers of obesity were necessary. This could look like restrictions on junk food advertising.
She commented: “Although taking steps to address obesity in the short-term is unlikely to have an immediate impact in the COVID-19 pandemic, it will likely reduce the disease burden in future viral pandemics and reduce risks of complications like heart disease and stroke.”
The study looked at hospitalised COVID patients from 18 hospitals, including China, America, Italy, South Africa and The Netherlands.