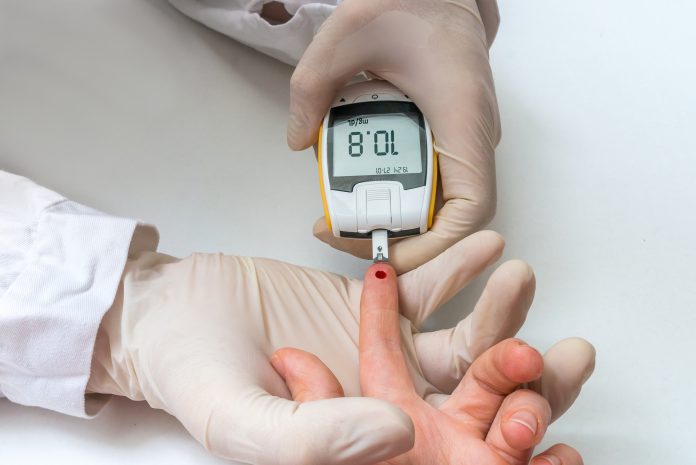
Here, a leading clinical negligence specialist warns the UK may be heading for a “perfect storm” of diabetes complications, due to delayed COVID-19 referrals
The UK may be heading for a “perfect storm” of diabetes complications, due to delayed COVID-19 referrals. We may be on the brink of a sharp rise in life-changing injuries due to diabetes complications being missed, as hospitals continue to contend with the chaos of the pandemic. Here, I explain how diabetes complications can quickly escalate, and how UK medics must be quick to refer patients; despite pressures mounting within the NHS.
Timely referrals: The difference between losing and saving a limb
Figures from the Office of National Statistics (ONS) reveal that almost 1,000 Brits died at home on a weekly basis from illnesses such as diabetes, cancer and Parkinson’s, in the period between March and September 2020 alone. Since lockdown began, the figure is up 26,000 year-on-year.
This is a shocking statistic and one that must be carefully considered.
It is crucially important for medical professionals to refer diabetes patients to the appropriate specialist at the first point of call; in order to avoid life-altering amputations that could otherwise have been avoided. The reduced number of available appointments means that potentially thousands of crucial referrals are being missed, which means we may be heading for a significant shift in catastrophic injury for those with chronic health conditions, such as diabetes.
As it stands, 169 avoidable amputations of “significant” severity occur each year in the UK due to diabetes referrals being missed, according to Diabetes UK – a number that is likely to have increased in 2020 and through to 2021.
People with diabetes are much more likely to suffer from health complications than the general population. Diabetics are two and a half times more likely to have a heart attack and twice as likely to have a stroke than a non-diabetic. Therefore, it is crucial that their condition is handled swiftly and correctly, to avoid any further difficulties. Unfortunately, this is not always the case.
Unfortunately, diabetes is growing in our society and it increasingly appears from a younger age. This places great demands on the health service, particularly at a primary care level.
GPs and hospitals have always needed to be vigilant to avoid a significant number of injuries caused by missed diabetes referrals, however, the challenges of the past year are highly likely to amplify this often-overlooked problem.
This issue is only likely to be exacerbated as the annual “winter crisis” tightens its grip, highlighting existing shortages and pushing our already-stretched resources to near breaking point, creating a danger that some may fall through the cracks. Medics must understand the warning signs of diabetes complications and act swiftly in the face of them. The sad reality is that this very often means the difference between saving and amputating a limb.
A medical professional’s duty
Diabetes is a lifelong disease which occurs when a person’s blood sugar is too high, affecting one in 15 people in England. Over time, having too much glucose in your blood can have significant consequences and so diabetics need to carefully manage and control their condition through medication and good care.
It is a medical professional’s duty to provide the care needed for a diabetic, and this is true even during the current climate. It is a concern that whilst pressures continue to mount within the NHS, the warning signs of diabetes complications will be missed entirely, or not seen until it is too late.
Medical negligence can occur through the treatment of diabetes when a healthcare professional does not provide an appropriate quality of care towards the patient. This most commonly happens when diabetes is misdiagnosed, if there is a delay in diagnosis or if treatment and care following diagnosis are not properly carried out. Patients are entitled to the appropriate care at all times, and it is important to remember this, even when circumstances are unprecedented.
Putting concern for the system before own health
Further research from the Fletchers’ Serious Injury department, conducted at the start of the pandemic, also revealed that a concerning number of the public would put off visiting a doctor should they require treatment. More than a quarter (26.8%) cited a reluctance to put an extra burden on the NHS – particularly important as hospitals currently contend with a second wave of COVID-19 – and a further 12.8% would be put off by a more general fear of visiting the doctors to receive care, which may lead to further crucial appointments being missed.
And this concern extends to patients delaying their own long-term treatment. Research revealed that half of those awaiting scheduled medical treatment have delayed their treatment themselves through fear of putting additional strain on the NHS – or through fear of contracting the virus.
This is particularly shocking, as around half of those who delayed their own medical treatment due to the pandemic, have seen their condition worsen as a result.
Imperative to remain vigilant
It is imperative that medical professionals remain alert to the complications of diabetes, and that those suffering long-term conditions such as this continue to attend scheduled appointments. It can all too often mean the difference between losing and saving a limb; a risk which when weighed against that of contracting the virus during a hygienic medical appointment, certainly comes out wanting.