Nordic countries are typically associated with high standards of living, high investment in the public health sector and low population density. Here, Biljana Stangeland PhD, analyses the drastic disparity in COVID-19 casualties between Norway and Sweden
Nordic countries experienced their first cases of COVID-19 late in February 2020. (1) The number of cases multiplied rapidly from the outset. (2) To deal with the COVID-19 outbreak, on the 12th of March 2020 the Norwegian government implemented drastic measures such as mandatory home offices, closed institutions, social distancing and restriction of public gatherings. On the 16th of March 2020, the country was officially shut down for travel. Denmark, Iceland and Finland implemented similar measures, while in Sweden, apart from few restrictions, life continued as normal.
What was the impact of lockdown?
In the time before and after lockdown, we kept monitoring the situation by calculating doubling times (DT) for COVID-19 cases in the Nordic countries. DT is a measure of the population growth.
Already one week after the March 2020 lockdown the positive effects were visible in several Nordic countries, (3) and two weeks after implementation the infection spreading was slowing. (4) The subsequential on-and-off lockdown regimes persisted for the whole of the 2020 and most of the 2021 in the Nordic countries except for Sweden, that based its strategy predominantly on recommendations, not restrictions. In the beginning of October 2021 and approximately 92 weeks after the outbreak, Norway, Denmark and many other countries finally abolished all restrictive measures.
Were the drastic and widespread measures effective and how did they influence Norway in comparison with Sweden that remained predominantly open throughout the whole epidemic?
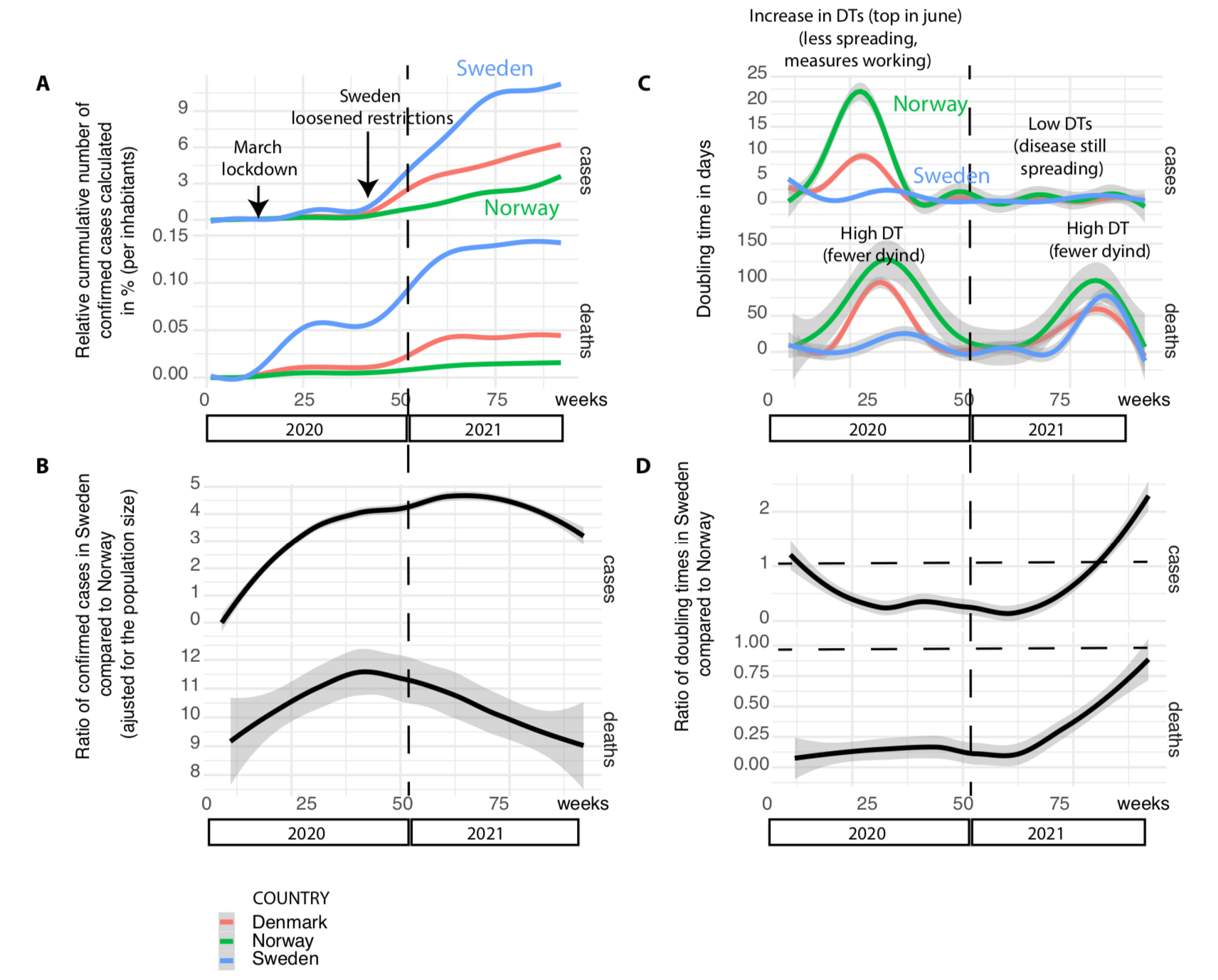
To answer this question, the number of confirmed cases and deaths in selected Nordic countries were assessed again (Figure 1A). According to ECDC (5) there were in total 1.16 million documented COVID-19 cases in Sweden, while more than 14,900 people lost their lives due to the disease. In Norway during the same period, there were 193,000 confirmed COVID-19 cases and 871 COVID-19 related deaths. Adjusted to the population size, the number of cases was five times higher in Sweden, and the number of COVID-19 related deaths was 12 times higher in Sweden than in Norway (Figure 1B).
To grasp how this enormous disproportion could happen we need to go back to the first lockdown and survey the number of cumulative cases and DT in Norway and Sweden for the period of 92 consecutive weeks from the outbreak in January 2020 to October 2021 (Figure 1C-D). In March 2020, the number of COVID-19 cases, calculated per inhabitant in Norway, was not so unlike that in Sweden and Denmark. (2,3,4,6) However, the situation started changing in April 2020 when it was obvious that the Swedish scenario was different to the Norwegian. (7) In spring 2020, Sweden experienced a higher increase in the number of cases than in neighbouring countries Norway and Denmark (Figure 1A). Sweden’s recommendation-based strategies and lack of will to embrace more draconian measures were to blame at least according to some experts. (8)
What is the lesson to be learned from the Swedish and Norwegian examples?
The general conclusion of many studies is that apart from the effects on the societies, the strict lockdowns, in periods, were effective in preventing the spread of the infection. Is this in accordance with the Nordic examples presented here? The examples of Norway and Sweden, two similar societies that chose different paths during the epidemic is very interesting. In 92 weeks after the outbreak the two, otherwise very similar, nations experienced tremendous differences, especially in number of COVID-19 cases and related deaths per inhibitor. The differences are evident, but is the explanation so simple? Why did things go so wrong in Sweden? Many of the Norwegian and Swedish experts have been wondering the same thing. (9) The scientific literature remains somewhat inconclusive. Can the mortality displacement explain the excessive Swedish deaths, as suggested by some scientists? (10)
Alternatively, could better routines in nursing homes have prevented many elderly residents from dying, as suggested by others? (11) Under interpretation of statistical data and overlooking important conclusions in fear of overstating that one thing causes the other in not unheard of. (12) The closest we come to a randomised real world scientific trial with COVID-19 viral transmission is an implementation of COVID-19 measured in two similar countries such as Norway and Sweden. We should restrain from hasty conclusions, but we cannot close our eyes to the overwhelming statistical data.
References
- Stangeland, B. https://www.dagensmedisin.no/artikler/2020/
03/12/tror-smitteveksten-er-underkommunisert/. Dagens medisin (2020).
- Stangeland B, https://www.dagensmedisin.no/artikler/2020/
03/12/70-dager-med-covid-19- -og-fortsatt-forvirret/. Dagens medisin, (2020).
- Stangeland, B. How to evaluate the success of the COVID-19 measures implemented by the Norwegian government by analyzing changes in doubling time. medRxiv, 2020.2003.2029.20045187, doi:10.1101/2020.03.29.20045187 (2020).
- Meadows, D. H. Thinking in Systems: a primer. (Chelsea Green Publishing Co, 2015)
- Stangeland, B. https://www.dagensmedisin.no/artikler/2020/
03/21/doblingstiden-har-doblet-seg- -er-det-grunn-til-optimisme/. Dagens medisin, online journal (2020).
- Stangeland, B. https://www.dagensmedisin.no/artikler/2020/
03/25/-mye-tyder-pa-at-stengte-skoler-og-hjemmekontor-virker/. Dagens medisin, online journal (2020).
- ECDC data repository for COVID-19 cases https://www.ecdc.europa.eu/en/covid-19/data.
- Stangeland, B. https://www.dagensmedisin.no/artikler/2020/
04/22/forsiktig-hap-etter-100-covid-19-dager/. Dagens medisin, online journal (2020).
- doi:10.1016/s0140-6736(20)32750-1 (2021).
- https://www.folkhalsomyndigheten.se/nyheter-och-press/
nyhetsarkiv/2020/oktober/viktigt-att-alla-tar-ansvar-nar-allmanna-rad-andras-for-personer-som-ar-70-ar-och-aldre/. (2020)
- Number of COVID-19 deaths by age groups (as of October 6, 2021) , https://www.statista.com/statistics/1107913/number-of-coronavirus-deaths-in-sweden-by-age-groups/. (2021).
- doi:10.1101/2020.11.11.20229708 (2020).
- doi:10.1016/j.jamda.2021.06.010 (2021).
- Amundsen, S. E. J. a. B. https://sciencenorway.no/covid19-health/why-did-things-go-so-wrong-in-sweden/1824724.
Sciencenorway.no, online journal (2021).
- Pearl, J. M., Dana. The Book of Why. (Penguin, 2019-05-02).
Please note: This is a commercial profile
© 2019. This work is licensed under CC-BY-NC-ND.