A report calls on the field of bioethics to look at racial injustice in the US, especially the impact of neoliberalism on contemporary health equity issues
According to the US National Institute of Health, bioethics is “the study of ethical, social, and legal issues that arise in biomedicine and biomedical research.”
The Hastings Center, which helped to create the field of bioethics, has released a compilation of work from an independent antiracism task force of bioethicists from across the United States.
Reflecting on the 50-year history of the field, the authors said that bioethics “has remained largely silent on issues of racial injustice.”
The field of bioethics needs meaningful, anti-racist change in science
Bioethics is vast, including concepts of medical ethics and environmental ethics, both of which split into intricate categories of functional, moral concern. When it comes to the contemporary advancements of science, tech and healthcare, there is a bigger and more urgent picture than just functioning outcomes.
The COVID-19 pandemic highlighted existing disparities in societies across the world. Universally, socioeconomic status was connected to likelihood of COVID hospitalisation and death.
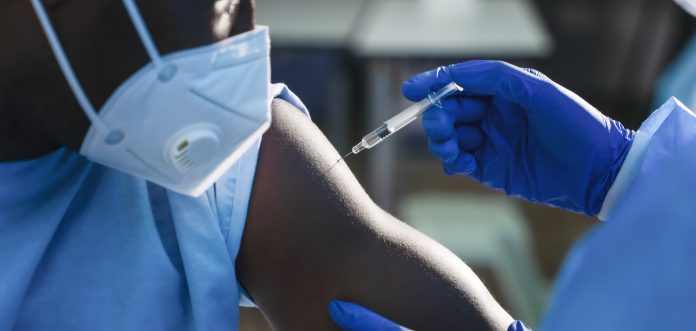
Even after the vaccination effect hit many countries in the Global North, people who work in lower-paid roles, experience existing immunocompromising illnesses or have less access to healthcare were more likely to experience severe illness.
Race was undoubtedly connected to these disparities, with ethnic minorities experiencing disproportionate rates of fatality.
In the UK, the first ten doctors to die of COVID were non-white.
In 2020, the rise of the Black Lives Matter movement brought fresh awareness to issues of anti-Blackness across the US. This consciousness spilled out from justice for victims of police brutality, expanding into other areas, such as health equity issues.
Authors reflect on issues like vaccine hesitancy and reproductive health
When it comes to neoliberalism, which includes such elements like the lessening of social safety nets and the privatisation of services, diminished healthcare outcomes were a direct consequence of changed priorities. The collaborative report looks at contemporary issues and overarching problems of health equity, such as the vaccine hesitancy of the Black community in the US.
Exploring how this hesitancy is often framed in a racist way, whether by healthcare professionals, journalists or individuals, Yolanda Wilson highlights a history of biological and psychological harm done to the Black communities of the US.
She writes: “The loss of loved ones, the loss of limbs, the loss of fertility—such things leave their mark on com-munities that experience them at the hands of institutions, whose harmful actions have often had the at least tacit approval of the government.”
Wilson further explains that asking questions is not “hesitancy”, but an instinct for information honed through a tenuous and violent history of mistreatment from authority figures.
Another article, written by Shameka Poetry Thomas, examines ongoing issues of maternal health for Black women by looking at how this group is pathologised and blamed for negative outcomes. Right now, Black women are three to four times more likely to die from preventable prenatal complications in the US.
She proposes the use of narrative medicine, “which involves listening to health narratives (or the patient’s lived experience)” instead of attempting to configure health experiences with that of white women, who are often the template for maternal biology.
Antiracism task force member, Dr Vanessa Y. Hiratsuka, said: “This special report is a call for structural change, a much-needed push to move from silent allies and activists within our trades, our professional organizations, our communities of practice, our communities of living, and our discipline communities —to uphold and uplift the values of justice and respect for persons within each of our communities and work toward being antiracists.”