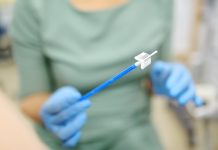
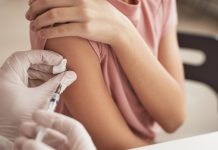
Dr Nighat Arif, a GP and Specialist in Women’s Health, argues that embracing women’s health data will re-shape preventative care
Those keeping an eye on proceedings at the UN General Assembly this year might have spotted the launch of an inaugural study into women’s health around the globe. Representing more than 2.5 billion women and girls worldwide, the Hologic Global Women’s Health Index was developed to understand how women’s life expectancy and quality of life can be improved.
Spearheaded by women’s health specialist, Hologic, in partnership with Gallup, it captures insights directly from over 60,000 women and girls in 116 countries and territories. Each country is given a ranking in the Index which considers five key areas of women’s health: preventative care, emotional health, opinions on health and safety, basic needs and individual health. That’s because these dimensions account for more than 80% of the variance in female life expectancy.
So, how did the UK fare? Overall, it ranked an impressive 12th in the Index – demonstrating strong leadership in women’s care, thanks to our unique universal healthcare system. However, when it comes to the preventative care dimension, it’s clear there’s work to be done, with the UK ranked 70th in the world.
Learning from the findings in the UK
In the UK, one of the most striking findings of the Index is that one in four women experience significant daily pain, rising to 38% for over 60s. While this finding is repeated across the globe, for me, it represents the tip of the iceberg in terms of the daily pain many of us live with. That’s because female pain is normalised in our society (and around the world) from an early age – usually, around the time girls start their periods. However, ignoring pain could mean women are missing the warning signs of serious health conditions such as heart disease or some cancers.
Women’s health is something the health service desperately needs to address. It is still under prioritised in too many areas of medicine, including in medical training, with topics such as the menopause – which impacts over 50% of the population – frequently only offered as short, elective modules.
Because of the way we, as a society, view women’s health, clinicians aren’t always attuned to the causes of female pain or early signs of illness, and women do not feel empowered to vocalise their concerns. When it is raised, female pain can often be taken less seriously, which means symptoms of ill health are more likely to be overlooked. For example, research has found that women who had a final diagnosis of a STEMI heart attack had a 59% greater chance of a misdiagnosis compared with men. (1)
This all combines to create an environment where preventative care becomes more of a challenge for women, with patients less likely to come forward and being met with a health service that’s not always able to understand and meet their needs when they do. Given women’s health is the cornerstone of healthy families, communities, societies, and economies, this is a problem that can no longer be overlooked.
Unlocking greater access to preventative care
The findings of the Index highlight the need for greater access to preventative care, identifying issues before pain is present, encouraging uptake of screening where it is offered and improving access to available treatments.
It’s essential that we help women better understand their bodies and their ‘normal’ as well as what they should be doing to remain healthy. This will empower them to take advantage of preventative care and to recognise pain and other signs of ill health, accessing medical help when they experience it. There is much to be done to achieve this, from finding ways to make screening procedures easier to access and as pain-free as possible, to equipping health professionals with a clear understanding of women’s unique challenges but, it is possible.
Reports like the Global Women’s Health Index are an important tool in supporting this goal. They give policymakers and healthcare leaders additional data around how they’re performing on women’s health and help them more confidently identify key strategic areas for improvement.
Embracing change
Triggering meaningful action will require cooperation from the government, the NHS, patient advocacy groups and industry. Initiatives such as the Women’s Health Strategy are a welcome first step on this journey. It is essential that we build on this momentum by championing women’s health, breaking down barriers to understanding and helping women to achieve a healthier, pain-free quality of life.
Having more joined-up commissioning of women’s health services and cross-departmental communication would be a helpful progression. The NHS is a fantastic, world-leading organisation that we should all be very proud of. Embracing change and directing funding to the areas that need it most, will allow it to evolve to better meet women’s health needs across the UK.
(1) Herrett E, Smeeth L, Walker L, Weston C. The Myocardial Ischaemia National Audit Project (MINAP). Heart. 2010; 96:1264-1267.