A new ‘white matter lesion’ mapping tool can find early signs of dementia, with more than 70% accuracy in measuring mental decline
Firstly, what are white matter lesions? Visually on brain scans, they are small bright spots on scans. These are called white matter hyperintensities, which are usually linked to memory loss and emotional problems. This becomes more common as people age, and can come with depression and strokes.
The white spots are usually fluid-filled holes in the brain, which are thought to come from a breakdown of blood vessels that normally nourish nerve cells.
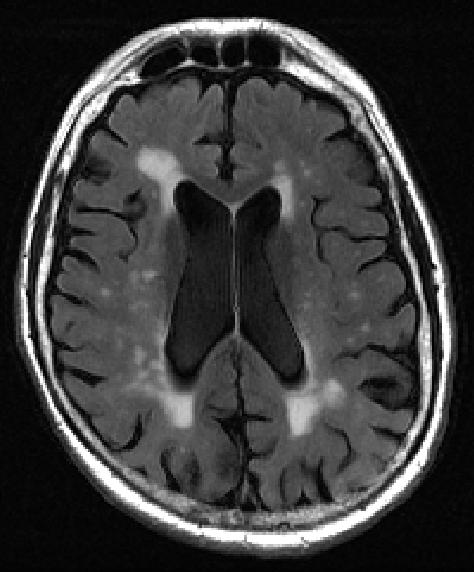
Researchers say that before this moment, finding and describing white matter hyperintensities in the brain depended largely on the “trained eye” – on a vague three-point scale. There is no uniformity to this – what could be a 1 (minimal) to one health professional, could look like a 2 or 3 to another. Calculations that concern life and death should not depend on visual subjectivity, especially when the clarity left to a dementia patient is ebbing constantly away.
“Amounts of white matter lesions above the normal range should serve as an early warning sign for patients and physicians,” says study lead researcher Jingyun “Josh” Chen, PhD, a research assistant professor in the Department of Neurology at NYU Langone Health.
Finding the new strategy, aka “bilateral distancing”
The NYU Langone team randomly selected 72 MRI scans from a national database of elderly people, the Alzheimer’s Disease Neuroimaging Initiative. They used equal numbers from elderly men and women who were mostly white, over the age of 70. The selected people had a mixture of normal brain function, mild cognitive decline, and suffering to severe dementia.
The researchers used computer software to calculate the precise placing and volume measurements for all observed white matter lesions – via MRI scanning to map the surface of the brain. What they did was to tabulate volumes (three-dimensional measurements in litres), based on each lesion’s distance from both side surfaces of the brain.
Normal ranges are between 0 millilitres (no lesions) and 60 millilitres (some lesions). Volumes greater than 100 millilitres suggested severe disease. When the researchers checked these measurements, they found that seven out of ten calculations accurately reflected the patient’s diagnosis.
Is it enough to change the future of dementia?
Chen cautions that the white matter brain measures alone are not sufficient to certify a finding of early dementia, but should be considered along with other factors – including a history of brain injury, memory loss and hypertension.
“Our new calculator for properly sizing white matter hyperintensities, which we call bilateral distancing, offers radiologists and other clinicians an additional standardized test for assessing these lesions in the brain, well before severe dementia or stroke damage,” says study senior investigator Yulin Ge, MD, a professor in the Department of Radiology at NYU Langone.
With a standardised tracking and measuring tool, it is now possible to monitor the growth of white matter lesions relative to that of other tau and beta-amyloid proteins also believed to be potential causes of dementia and Alzheimer’s disease. The build-up of either substance could also prove or disprove one or more of the theories about what biological processes actually lead to various forms of dementia.
Crucially, healthcare professionals can use the tool for free right here.