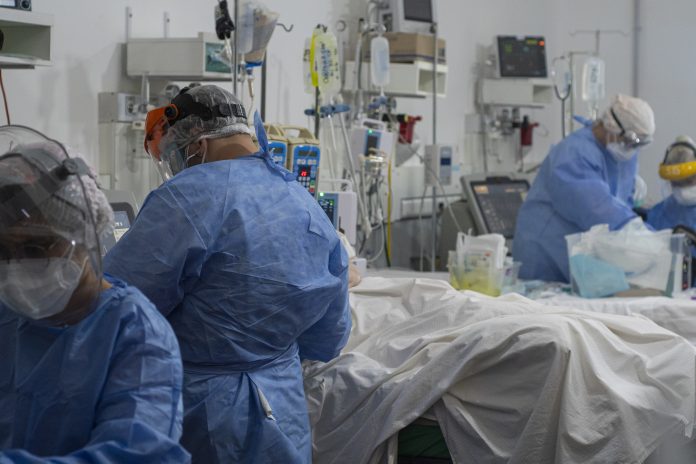
Scientists describe COVID pneumonia as “multiple wildfires spreading across a forest” – but how different is the condition from regular pneumonia?
A study in The Lancet Rheumatology finds that 20% of people infected with the virus suffer from COVID pneumonia, needing hospitalisation.
Ordinary pneumonia, the swelling of tissue in one or both lungs, is caused by a bacterial infection. According to the NHS, symptoms can develop over 24 to 48 hours, or even take several days.
With pneumonia caused by COVID, the inflammation is created by the virus, and takes a different form.
Is COVID pneumonia different to ordinary pneumonia?
Yes. It lasts for longer and creates more multiple-organ complications.
A team at Northwestern Medicine had a chance to directly analyse lung fluid from hospitalised COVID patients. They found that COVID pneumonia is different to ordinary pneumonia, after comparing lung immune cells to pneumonia samples collected before the pandemic.
COVID pneumonia hijacks immune cells in the lung, using them to spread across the organ over a period of days or weeks. While ordinary pneumonia infects large regions of the lung, COVID takes over multiple, smaller areas of the lungs.
The scientists described this lung takeover as “multiple wildfires spreading across a forest.”
Infection then travels slowly across the lung, damaging breathing capacity, then fuelling the fever, low blood pressure and damage to every organ in the body. Hospitalised patients face complications because of how long the disease takes, not because COVID pneumonia is an intrinsically more severe disease than regular pneumonia.
Which people are most likely to get this kind of pneumonia?
People with diabetes, moderate to severe asthma, lung disease, high blood pressure, heart disease, liver issues, and cancer.
Basically, this health outcome is likely for anyone who already deals with an illness that puts oxidative stress on the lungs, increases likelihood of inflammation or has a lowered immune response is at high risk of experiencing the kind of COVID pneumonia that leads to hospitalisation.
A study published in September, 2021, finds that diabetes is the “main medical problem” associated with COVID-19 globally. The authors, mostly at The Hamadan University of Medical Sciences in Iran, said: “It is plausible that diabetes can forecast elevated severity of pneumonia. The mortality of lung infection among diabetes is remarkably higher compared with non-diabetic patients.”
Diabetes is also strongly linked to socioeconomic disparity and race, meaning that a certain demographic of people are more likely to end up hospitalised with severe COVID.
How long does it take to recover from COVID pneumonia?
Up to one year for a minority of people, but more studies are needed to understand the long-term effects.
In research conducted by The Radiological Society of North America in March, 2022, a team found 63% of patients with chest abnormalities did not show further improvement after six months. They also realised that men, patients over the age of 60, and those with critical COVID severity were most likely to have lung issues – even after one full year from the point of infection.
Contrary to this, an earlier study in 2021 found that one third of patients’ lung function remained reduced, even a full year after the experience of virus-related pneumonia. Despite the findings of The Radiological Society, in this study, loss of lung function was more common in women than in men.
Dr Mark Jones, Associate Professor in Respiratory Medicine at the University of Southampton and co-leader of the second study said: “The majority of patients with severe COVID-19 pneumonia appeared to fully recover, although for some patients this took many months. Women were more likely to have persistent reductions in lung function tests and further investigation is needed to understand if there is a sex specific difference in how patient’s recover.
“We also don’t yet know what happens beyond 12 months and this will need ongoing study.”