Dr Christine Wekerle from McMaster University discusses youth health risks and why resilience is crucial to youth wellness
Adolescence is a time of risk and resilience. Supporting wellness is a priority for youth involved in child welfare or care systems. Over 400,000 youth are in care homes in the United States, and their trajectory in exiting care needs to set youth up for success. Led by Dr Christine Wekerle at McMaster University, with an interdisciplinary research group, the Maltreatment and Adolescent Pathways (MAP) study was the first large-scale Canadian study of youth in an urban child welfare catchment area. Unexpectedly, MAP youth reported more child sexual abuse (CSA) than anticipated by agency statistics. For youth, engaging in health risk behaviours, like risky sexual practices (Wekerle et al., 2017) or alcohol use, highlight a need for supporting healthy coping (Park et al., 2019; Hudson et al., 2015; Hudson et al., 2017; Goldstein et al., 2011; Stewart et al., 2011). Resilience interventions are needed to support youth in building adaptive daily routines. Maltreated youth have significant resilience; their route to thriving means galvanizing their resilience. A team of Canadian researchers are taking up the challenge of how to support child welfare youth.
Trauma, alcohol problems and coping methods
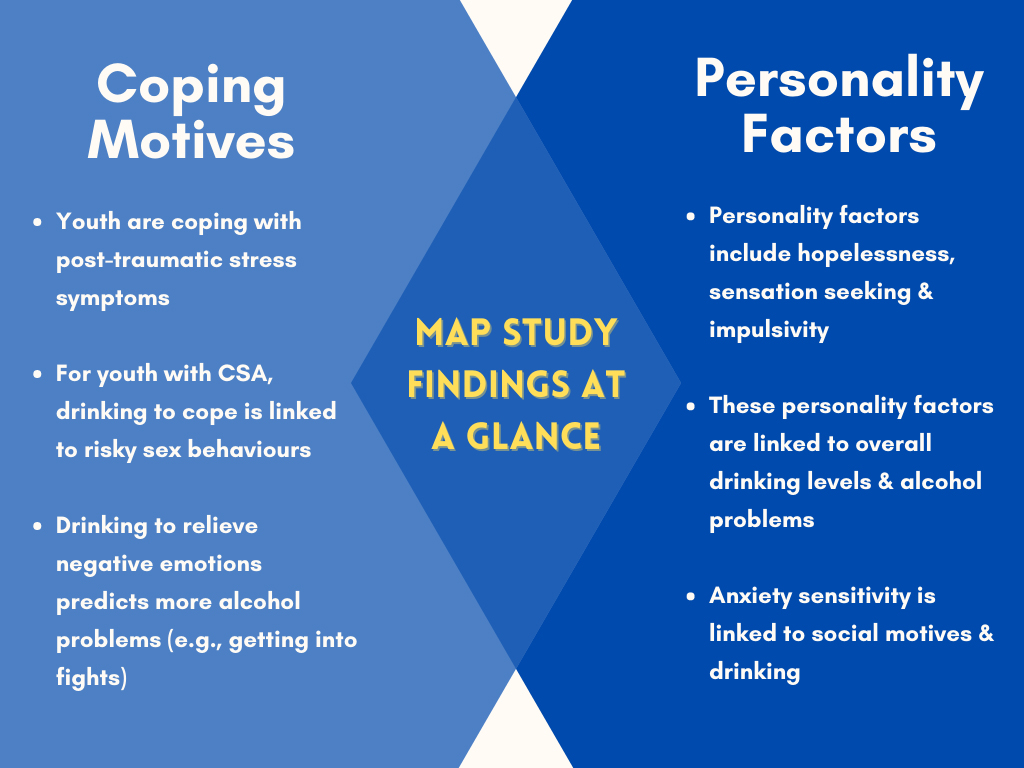
While the legal age of drinking in Ontario, Canada is 19 years of age, MAP study youth (mean age 16), who reported higher traumatic stress initially, were more likely to report drinking to cope six months later. The motive of drinking to cope predicted higher alcohol use. This may reflect the beginnings of a self-medication cycle, where alcohol use may provide temporary relief, but could amplify trauma symptoms, like hyperarousal, with the agitation feelings of withdrawal. Real-time help, that can respond to variations in symptoms, may bolster the regulation of emotions. Mobile applications (apps) are an easy-to-access potential solution. However, research shows that only a minority of mental health apps identified their research basis or involved mental health expertise in their design (Marshall et al., 2019). The MAP research shows that the key issues impacting youth alcohol use are post-traumatic stress and anxiety symptoms (Park et al., 2019). As summarised in the table, MAP findings point to the need to address maladaptive coping. In response, our team developed the JoyPopTM mobile app, designed to enhance resilience, using research on effective emotion regulation methods (see youthresilience.net). JoyPopTM is a trauma-informed app that prioritises youth safety and privacy. JoyPopTM puts a focus on awareness of positive emotionality and joyful activities, while providing traumatic stress management strategies. The Ontario Centre of Excellence in Child and Youth Mental Health is funding current research examining the response to this app among child welfare system-involved youth, with lead researcher Dr Deborah Goodman from the Child Welfare Research Institute in Toronto, Canada.
Adolescent personality vulnerabilities also play a role in maladaptive coping. Chronically feeling hopeless, tending towards seeking stimulation and impulsivity are all linked with overall alcohol use levels and alcohol problems (Hudson et al., 2015; Stewart et al., 2011). Feeling sensitive or fearful to signs of anxiety, interpreting them as threatening, is related to difficulties with stopping drinking once having started. Trait-like hopelessness and impulsivity are most closely linked with negative emotions and drinking to cope among MAP youth. For youth high on anxiety-sensitivity, motives for drinking are more likely to be related to the need to avoid social rejection. Brief, cognitive behaviour therapy that matches skill development to these specific personality vulnerabilities has an impressive set of research studies supporting decreased substance use, sustained over time. This Preventure intervention, created by Drs Patricia Conrod and Sherry Stewart, is currently being tested with child welfare-involved youth, in collaboration with Dr Hanie Edalati. Based on the Preventure model, the Well-Venture adaptation takes a trauma-informed approach (Edalati & Conrod, 2019). Currently underway in Montreal, Canada, pilot work shows that a third of youth had diagnoses for PTSD and used cannabis on a daily basis (Edalati et al., 2020).
The impact of child sexual abuse
For youth who have experienced CSA, the MAP study points to specific sex differences in coping strategies and motives. CSA and problem drinking was explained by negative emotion symptoms more so in female adolescents than males (Wekerle et al., 2017). For males, greater sexual risk-taking was noted. Males with CSA experiences reported their motives for having sex as including seeking peer and partner approval and coping with negative emotions. For both MAP males and females, coping was a key mediator between their maltreatment and sexual risk-taking.
Altogether, the MAP study points toward the need for more accessible, trauma-informed support for youth negative emotionality (Bargeman et al., 2020). The COVID-19 pandemic puts another layer of traumatic stress on youth experiencing trauma. Among Canadian youth, 23.6% reported drinking face-to-face with peers during the pandemic, particularly among youth who perceived themselves as less popular (Dumas et al., 2020). More attention to youth motives for risk behaviours is needed to support maltreated youth. Research on resilience programming is critical to advance science-based policy. Our youth in care deserve the best opportunities for success, including the resilience resources to achieve success. Reaching out is resilience, but those adaptive coping resources need to be readily available to youth in such risk contexts.
Acknowledgement: We thank the support of our funders and trainees, particularly Katherine Kim, Corinne Moss and Jung Yoon (Jane) Park. CSA research was funded by a Canadian Institute of Health Research, Institute of Gender and Health team grant (Dr Wekerle lead, CIHRTEAMSV).
Please note: This is a commercial profile