Over 350 million people suffer from arthritis pain globally, which means significant levels of opiates are used to manage the condition – but what if there was a less addictive treatment?
A research team have found a treatment that could reduce reliance on addictive opiates, which would help with severe arthritis occurring in hip and shoulder joints.
The pain that happens to people suffering with arthritis is often severe, with very few cohesive treatment options. Injecting anaesthetic and corticosteroids into the joints themselves is a classic strategy – but this gets less and less effective over time, as the disease gets stronger than this medication.
Felix M Gonzalez, MD, from the Radiology Department at Emory University School of Medicine in Atlanta, Georgia, said: “The first anesthetic-corticosteroid injection may provide six months of pain relief, the second may last three months, and the third may last only a month. Gradually, the degree of pain relief becomes nonsignificant.”
Without pain relief, patients face the possibility of joint replacement surgery. Many patients are ineligible for surgery because of health reasons, whereas many others choose not to go through such a major operation. For those patients, the only other viable option may be opiate painkillers, which carry the risk of addiction.
Cooled radiofrequency ablation (c-RFA), aka ‘stunning’ the joint
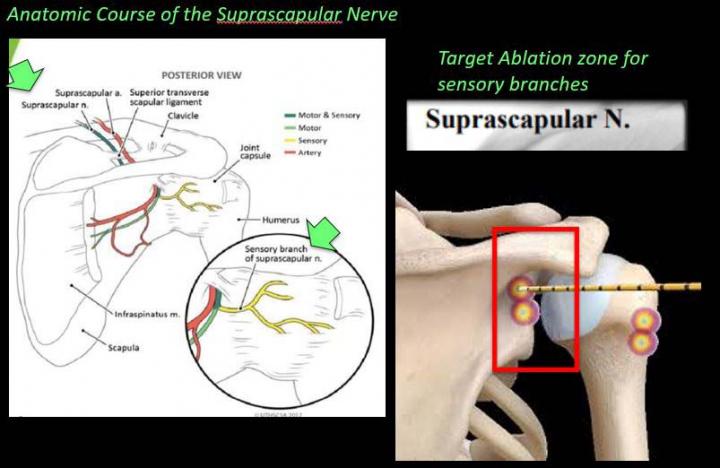
This research was presented at the annual meeting of the Radiological Society of North America (RSNA). Dr Gonzalez and his colleagues have been working with the use of a novel radiology treatment, cooled radiofrequency ablation (c-RFA), to achieve pain relief. This means that needles are placed around the main sensory nerves in shoulder and hip joints. The nerves are then hit with a low-grade current known as radiofrequency, which is how they’re ‘stunned’. This stunning slows the journey of pain to the brain, making the condition more bearable without any drug ingestion.
The research team chose 23 people with osteoarthritis to undergo treatment, including 12 with shoulder pain and 11 with hip pain that had become unresponsive to anti-inflammatory pain control.
The treatment was performed two to three weeks after the patients received diagnostic anaesthetic nerve blocks. The patients then completed surveys to measure their function, range of motion and degree of pain before and at three months after the ablation procedures.
What did the research team find out about arthritis pain?
“In our study, the results were very impressive and promising,” Dr Gonzalez said.
“The patients with shoulder pain had a decrease in pain of 85%, and an increase in function of approximately 74%. In patients with hip pain, there was a 70% reduction in pain, and a gain in function of approximately 66%.
“This procedure is a last resort for patients who are unable to be physically active and may develop a narcotic addiction. Until recently, there was no other alternative for the treatment of patients at the end of the arthritis pathway who do not qualify for surgery or are unwilling to undergo a surgical procedure.”
“We’re just scratching the surface here,” Dr Gonzalez further said. “We would like to explore efficacy of the treatment on patients in other settings like trauma, amputations and especially in cancer patients with metastatic disease.”