Mr Mbayo Guy Kakumbi, Technical Officer and Dr Bagayoko Magaran, Senior Scientist from The World Health Organization (WHO) Regional Office for Africa reveal their stance on the essential global resource of water
Human society depends on biodiversity – the variety and complexity of life on earth – to provide food and medicine. Human existence and activity on earth are tributaries to the availability of water to ensure vital productivity functions, such as agriculture, industry, energy, transport and environmental biodiversity.
Water is indeed essential for life.
The uneven distribution of fresh water is becoming one of the most important global resource issues. The availability and quality of water resources are key to alleviating poverty and the growth of societies. Social progress rests on economic development. This, in turn, depends on energy, for which the world’s demand continues to grow year by year. It is principally about wealth creation and managing this efficiently will provide critical value for future generations.
Bacteria, viruses, parasites and fungi (including mushrooms) are microorganisms that can induce diseases and are known as pathogens. These lower forms of life can be causative agents for certain diseases, that is, bacteria (classical waterborne diseases, for example, cholera, typhoid), viruses (smallpox, yellow fever, the common cold), animal parasites: protozoa (amoebae, plasmodia), helminths (hook/tapeworms, blood/liver flukes) and fungi (athlete’s foot).
Protozoa are a large collection of organisms with considerable morphological and physiological diversity; they are found in almost every aquatic environment and are widely distributed. They play an important role in all aspects of sanitary microbiology ranging from their health impacts as human pathogens and through to their role in the treatment of potable waters and wastewaters.
Infection is the invasion of the host by some other form of life followed by the growth and multiplication of the invading organism within the body of the host.
Soil, animals and humans can be reservoirs that carry infections. The avenues for escape could be respiratory tracts, urinary tract, digestive tract, open wound or mechanical escape by blood-sucking insects. Transfer of infection could occur by direct transmission (man-to-man) or by indirect transmission through animate (vectors) or inanimate (fluids, air or soil) vehicles.
Portals of entry to the new host are usually respiratory tracts, percutaneous entry (via a bite, for rabies or malaria); direct penetration of the skin by causative agents (e.g. hookworms, schistosome cercariae), gastrointestinal tract (ingestion of contaminated food or drink) and direct infection of membranes.
Disease will effectively follow in the host only according to the level of vulnerability – resistance and immunity of the host.
Whilst “better water and sanitation were associated with an improved rate of linear growth and a decreased risk of diarrhoea” (The Lancet, 2004), in Africa, diseases caused by pathogenic microorganisms associated with water are the most important as they cause more deaths and illnesses.
Proliferation of these microorganisms in the environment due to poor handling of the environment (inadequate sanitation leading to contamination of fresh water, desertification and soil erosion leading to diminution of lens of fresh water or chemical spill leading to pollution of fresh water stocks) is very likely to induce lack of sufficient safe water especially considering the current of population growth.
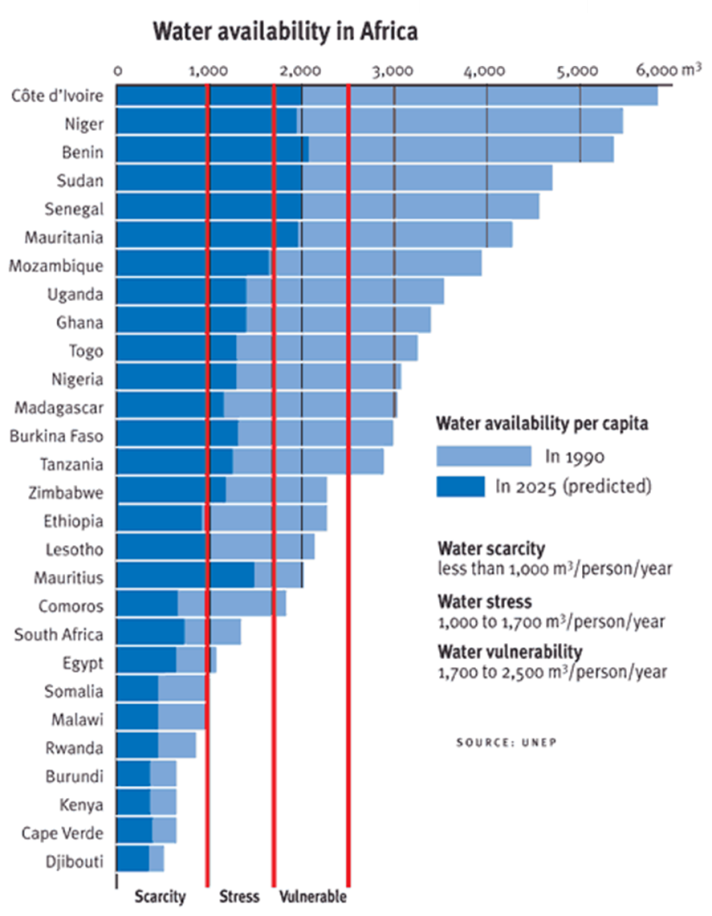
Water scarcity is assessed by the national availability in a country of an average of less than 1000 m3 per capita per year to meet all life water needs (see figure 1 above). Sub-Saharan Africa counted the greatest number of water-stressed countries in 2006 with up to 300 million individuals being affected.
To sustain life, people will have no choice than to resort to unsafe water sources. More often, people tend to store water in their dwelling, increasing the risk of poor water handling that occasion bacterial contamination and better breading of vectors, such as mosquitoes responsible for malaria or dengue fever.
The report on “Water scarcity in Africa: issue and challenges” anticipated that the situation will worsen his with between 75 to 250 million people expected to reside in high water-stressed areas by 2030 with the potential to create displacement and the cohort of problems that come along. Despite being at the same time, the most lethal, treatable and preventable, most water-borne illnesses are also the major common disease to affect Africans especially their infants, children and women.
Water scarcity has a huge negative impact on health, on hygiene, on economic productivity as they also hijack resources that could be used for other purposes for the sake of treating these water-borne diseases; this undermines countries harmonious development but perpetuates poverty.
The gender division of labour usually practiced in the Africa region put women and girls at disadvantage compared to men. The latter group is not usually responsible for the collection, management, and the safeguard of water, especially at the household level. By carrying these heavy loads made of jerrycan full of water as women and girls do over long distances on daily basis, adverse health consequences fall upon them, such as permanent skeletal damage which leads to more stress, more time needed for recovery from illnesses, and less time and ability to attend school.
According to UN Environment, out of 2.5% of fresh water that exists in the world, groundwater makes up for at least 30.8% whilst lakes and rivers, 0.3% and the remaining 68.9 % are locked into glaciers.
Hygiene education seeks to alter inappropriate beliefs and practices by communicating the right messages in an appropriate way. Hand washing with soap reduces water-washed diseases and acute respiratory infections (ARIs)
[Cairncross, 2003]. Hygiene is a vital issue which was missing from the MDGs framework and which is tackled under SDGs in the post-2015.
Diarrhoea is still the most important public health challenge at the moment. It is the major reason of death up to the age of 15 years, whilst the five first years of life are the most at risk. Repeated diarrhoea (and heavy parasitic infection) in infancy leads to stunting (= low weight-for-age) and, very importantly, to poor cognition in later childhood [Berkman et al, The Lancet, 2002].
23% of all deaths in Africa are linked to the environment. That’s 2.2 million people. On a per capita basis (deaths per 100,000 people), Africa is the region with the highest burden of deaths in the world. Environmental impacts on health are uneven across age. 26% of children under five and 25% of adults between the ages of 50 and 75 died prematurely from environment-related causes.
According to the WHO-UNICEF joint monitoring programme report 2017, 669 million people did use an improved drinking water source 26% of people in sub-Saharan Africa use safely managed water services representing some 257 million as of end 2015. At the same time, 695 million people in the Sub-Saharan Africa region did not have access to improved sanitation facilities – 217 million of whom practiced open defecation.
In 2015, 404 million people (40%) in the African region (AFRO) lacked a basic drinking water service. 83.3% of the urban population and 43.7% of the rural population used a basic drinking water service. At the same period, some 687 million people (70%) in the African region lacked a basic sanitation service with 216 million people practicing open defecation. 44% of the urban population and 21.4% of the rural population used a basic sanitation service.
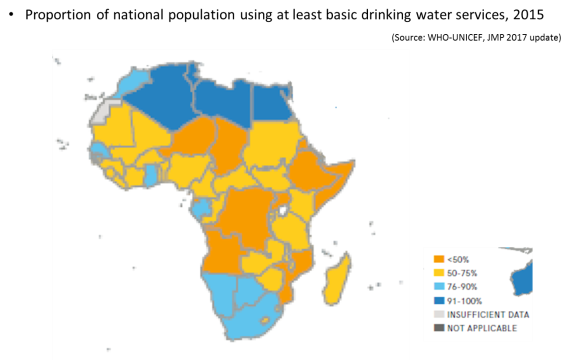
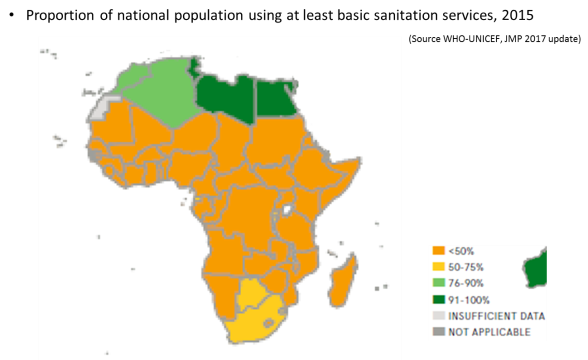
When the millennium development goals (MDGs) era started, target 7.C was set for countries to halve, by 2015, the proportion of the population without sustainable access to safe drinking water and basic sanitation. In 1990, 48% of people living in sub-Saharan Africa had access to improved drinking water sources and the global MDG target for drinking water was met five years ahead of schedule. In the other end, in 1990, the proportion of people using an improved sanitation facility in sub-Saharan Africa was only 24%.
Climate change is expected during this century to lead to a temperature rise between 1.8 to 4.0°C; in the worst case scenario, it can raise up to 6.4°C depending on how quickly and drastically the world manages to reduce carbon emissions by deeply modifying its production and consumption patterns. The increase of global mean temperatures will lead to a change in global climatic patterns and consequently, in regional and local water balances. The clearest predicted impacts are an increase in the variability, intensity and frequency of floods, droughts and extreme weather events.
However, the impacts of climate change on water, sanitation and hygiene go beyond floods and droughts and include:
• Adverse impacts on water quality and availability;
• Increased water stress;
• Changes in groundwater recharge patterns;
• Greater rates of erosion;
• Increase landslide-associated casualties and;
• The poor performance of sanitation systems, leaving the population with no sanitary protection.
This state of affairs will certainly exacerbate water scarcity impact considering projected population growth in general, and migration of population towards urban settings. The majority of the world’s children will soon be living in urban areas – in Africa like in Asia, most of these in slums. The pace of urbanisation is so fast that intervention design often cannot keep pace with implementation especially if there are already evident infrastructure gaps as in most African cities today.
To mitigate all the above, Water Safety Plans (WSPs) were ¬first introduced by WHO through the 2004 Guidelines for Drinking-water Quality as the most effective means of consistently ensuring the safety of a drinking-water supply.
WSPs require a risk assessment, encompassing all steps in water supply from catchment to consumer, followed by implementation and monitoring of control measures. WHO partnered with many organisations (such as the International Water Association, UNICEF and others) to organise series of training on this approach for Member States staffs across the continent.
To date, several pilot projects are carried out in Senegal, Ethiopia, Liberia and Ghana in order to contextualise and crystalise this strategy.
References
1. http://www.un.org/millenniumgoals/2015_MDG_Report/pdf.
2. Accessed on 12/02/2019.
3. WHO-UNICEF Joint Monitoring programme 2017 report.
4. Course note Tropical Public Health: Diarrhoea, Leeds University.
5. WHO website, Fact sheets: tropical diseases.
6. Conference on water scarcity in Africa: Issues et Challenges, 2016.
Dr Mbayo Guy Kakumbi
Technical Officer
Dr Bagayoko Magaran
Senior Scientist
The World Health Organization (WHO)
Regional Office for Africa
Tel: +(47 241) 39402
Email: afrgocom@who.int
Website: www.afro.who.int
Twitter: https://twitter.com/WHOAFRO











