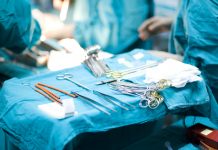
Dr. Jo Gee writes about working with personality disorders through her psychotherapy experience of over 10 years: Read on for what she has to say about mental health treatment
What is a personality disorder (PD)?
It’s often defined as a way of thinking, feeling and behaving that deviates from what is considered normal, causing distress and problems with general functioning.
The difficulties experienced by someone with personality disorder are long-standing and although the symptoms will vary depending on the type of personality disorder, all PDs have in common:
- distorted thinking patterns
- intense or problematic emotional responses
- difficulties with impulse control
- difficulties in interpersonal situations
In order for a diagnosis to be made, significant and enduring difficulties must be experienced in at least two of the four categories.
Borderline personality disorder
Borderline personality disorder (BPD), which emerges from an interaction between genetic and environmental factors, is a disorder which affects mood, emotional responses and interpersonal relationships. Those with BPD generally experience emotional dysregulation, which involves intense mood changes, which are not easily regulated, disturbed patterns of perception, impulsive behaviour which often includes self-harming behaviour and unstable relationships.
Experience working with personality disorders
I have worked with personality disorders for over 10 years, in the NHS, private hospitals and forensic settings, and one of my most important learnings is that bespoke treatments for BPD are efficacious and have a huge effect on the symptoms experienced by the person with BPD. In fact after 12-18 months of treatment, many of my patients no longer meet criteria for a personality disorder, experiencing changes to their perceptions, an ability to regulate their emotions and the ability to manage impulsive behavioural urges.
Over the last 15 years, evidence has emerged which shows that psychological treatments can effectively treat PDs (Bateman and Tyrer, 2004), addressing features of BPD including impulsivity, emotional dysregulation and self–harm.
But the therapeutic work isn’t always easy. The therapy can feel like crisis management, as at the beginning of treatment, the person with the personality disorder often presents with suicidal feelings, self-harming behaviours and intense emotions. The level of anxiety this brings up in the patient and therapist is great, and it requires firm therapeutic boundaries on which the therapy is built.
Interpersonal issues also play out within the therapy itself. The person with BPD may present with the perception of being rejected and persecuted by others, and this can be easily felt towards the therapist, at the end of the sessions, in holiday breaks, or in something the therapist said that the patient felt was rejecting.
Therapists often experience being idolised, and then swiftly demonised due to something experienced by the person with BPD within the sessions; even if this ‘something’ is perceived by the therapist as irrational.
Therapists often experience being idolised, and then swiftly demonised
This can easily lead to burnout of the therapist, and breakdown in the relationship. I often treat patients for BPD who have engaged in conventional counselling or psychotherapy, and experienced a therapeutic fallout which felt damaging to them, and within which, they didn’t progress.
A way forward
As stated, people with BPD can experience immense changes to their life by treatment end, which at treatment start, they are unable to envisage. Yet in order to get there, a specific treatment regime is required.
This is why, in my personal experience, generic counselling and psychotherapy is not suitable for the treatment of BPD. The NICE guidelines do not recommend generic, brief psychological interventions. The guidelines also recommend that any treatments for BPD need to include:
- an explicit theoretical approach, shared with the patient
- structured care
- provision for therapist supervision
- frequency of 2 sessions weekly considered
Further, when BPD includes recurrent self-harm, they suggest Dialectical Behaviour Therapy (DBT) as the gold standard treatment for BPD. DBT has a vast evidence base for BPD (Linehan et al., 1991; Linehan et al., 2006; Linehan et al., 2015).
In my work, I have found DBT to be highly effective, providing a stable and safe structure for therapist and client. A structure which is clear, provides firm but thoughtful boundaries, and has offers techniques, strategies and rules to help prevent and manage interpersonal issues and boundary breaks.
What is DBT?
DBT is a cognitive behavioural therapy created specifically for BPD by Marsha Linehan, which draws on the idea of the dialectic, which is the study or inquiry into opposites. Dialectical strategies support both therapist and patient, to synthesise views and become unstuck from extremes, which are inherent in BPD.
Goals are also vital in DBT treatment planning, in ensuring that the symptoms are targeted. The behavioural aspect involves assessing and targeting behaviours, in order to solve problems through teaching the client skills which helps them reach these goals. However, it’s important to note that in helping clients develop a life they see as worth living, the therapist needs to help them work to the goals defined by them.
Even the core assumptions of DBT support the work, by helping the therapist view clients in the best light. The therapist needs to maintain compassion for the client and their difficulties in emotional regulation, whilst also understanding it’s the client’s role to solve their problems in the now, even if they weren’t the original cause of their suffering.
There are four modes within the DBT treatment:
- Individual psychotherapy
- Skills training
- Phone coaching
- DBT consultation, a structured programme of supervision and reflection for therapists
These modes all make up a structured, effective treatment with a strong research base.
Therapist support working with BPD
One of the most important areas of the work with BPD is ensuring the therapist is supported so that they don’t burn out, whilst remaining compassionate and effective as practitioners. This is where the DBT consultation is so important.
Within the DBT consultation, practitioners within the team working with clients take up different roles, helping each other manage the stress of working with high-risk clients. The consultation team helps to enhance therapists clinical skills, monitor fidelity to the treatment model and ensures the therapist maintains their balance by walking the path of acceptance of the clients difficulties, and the need for change with regards to behaviours and responses.
Forward-thinking
In the community, work with BPD takes place under a multi-disciplinary team, where psychiatrists, care coordinators and mental health teams pay an important role. This is an important aspect in ensuring effective treatment.
Moving forward, headway has been made with ensuring appropriate treatments are available for people with BPD. However we need to further improve provision. At present, the criteria for a person receiving DBT in the community is judged mainly on how high risk they are. This makes sense to some level, but often means that people with BPD are offered more inappropriate treatments, such as CBT or generic counselling, only being offered DBT or a similar evidence-based treatment when their symptoms progress and they reach crisis point.
We have effective treatments, which help to keep the therapist and client safe, and bring about real behavioural change. And it’s these treatments we need to make sure are available.
By Dr. Jo Gee, a Psychotherapist
Editor's Recommended Articles
-
Must Read >> Insights: The seven year pain of Endometriosis
-
Must Read >> Insights: Life after an HIV-positive diagnosis