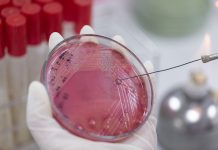
David Partridge from the British Infection Association provides a comprehensive overview of effective infection prevention and control in the UK today
In 1967, US surgeon-general William Stewart proclaimed, “It is time to close the book on infectious diseases. The war against pestilence is over.” 50 years later, healthcare-associated infection is estimated to cost the NHS £1 billion per year. What Stewart underestimated was the extraordinary ability of microbes to adapt to their environment and the power of natural selection to ensure that favourable genetic traits evolve and are propagated. With an acceptance that we cannot simply develop new drugs to obliterate any pathogen, the speciality of ‘infection prevention and control’ has become our front-line defence.
Effective infection prevention and control relies on:
- Identification of an infection risk, either human or environmental;
- Understanding the mode by which that infection may be transmitted to patients and;
- Implementation of interventions to remove the risk or interrupt transmission.
MRSA
To illustrate this, we can reflect on our successful efforts to reduce the burden of Meticillin-Resistant Staphylococcus aureus (MRSA) with bacteraemia rates in England and Wales falling by 82% since 2007. For MRSA, risk identification was facilitated by predictable epidemiology and easy, accurate screening tests and management by interventions such as enhanced cleaning, antibiotic stewardship, alcohol hand gels and barrier nursing plus the possibility of eradication therapy for affected patients, and alternative treatment options for those with established infection. Equally vital was public recognition of the problem and consequent political pressure for action which ensured that appropriate resources were dedicated to tackling it.
The same focus is now required on other, more formidable foes. Carbapenemase-producing Enterobacteriaceae (CPE) are resistant to nearly all current antibiotics and have emerged rapidly over the past decade, such that over 2500 such organisms were referred to the Public Health England in 2016. CPE and similarly resistant germs threaten to reverse the huge medical advances that have been supported by antibacterial therapy, not least in ensuring the safety of surgery and of anti-cancer chemotherapy.
Other organisms, such as Middle East respiratory syndrome coronavirus have the capacity to result in high mortality outbreaks if imported and then unrecognised and not contained. More familiar viral infections such as norovirus and influenza still close countless hospital wards each winter.
Diagnostics
Diagnostic laboratory provision has a major bearing on control of infection and the best model for the UK is currently the subject of debate. NHS improvements suggested hub and spoke model of pathology services has recently been published with the £200 million carrot from Lord Carter’s report on healthcare efficiency, but any real savings need to be built on the foundation of effective transport and IT links between laboratory and bedside.
Without these fundamentals, diagnostic delay and resultant sub-optimal decision-making is likely to result in inappropriate resource use or breakdown of infection control strategies. Point of care testing with molecular diagnostic devices can provide rapid results for organisms such as MRSA and influenza. These tests currently cost more than existing laboratory-based methods but
the benefits of more timely results may mitigate some of the problems related to off-site laboratory provision as an increased repertoire of tests becomes available.
When infection control risks are present, healthcare facilities must resist the transfer of relevant organisms between patients, staff and the environment but this must be balanced against a need to ensure that the patient does not have their care or mental well-being unnecessarily compromised. This is a particular challenge in community healthcare where the facility is also the patient’s home.
Comforts such as carpeted floors have long been eliminated from hospitals due to their potential to harbour infection, but their removal from residential care is much more contentious. Infections related to medical devices, especially urinary catheters, are a major burden in both hospital and community.
Smart materials may be employed in both patient devices and the environment. Surfaces which resist the development of biofilms (slime encased microbial communities), may coat orthopaedic implants or protect against infection of intravenous lines and urinary catheters. On a wider scale, high contact point surfaces in the hospital environment such as commodes and toilet door handles should be designed to resist contamination or to provide some indication that they have a significant level of organic soiling, such that cleaning time can be targeted more effectively.
NHS resources
In addition to the human misery caused by infection control threats, they and the measures introduced to prevent them have an enormous operational and financial impact on the NHS. Added to this, our era of budget restraint mandates that we attempt to reduce this drain on scant resource.
The challenge for policymakers and infection prevention and control providers is identifying interventions which achieve the greatest benefit for each pound spent. This task is complicated by the fact that, like other safety disciplines, the obvious outcomes tend to be failures as it is rarely possible to measure infections prevented as they haven’t happened!
During the West African Ebola outbreak in 2014-15, trusts put significant resource into education, policy development, diagnostic strategies and isolation facilities. As a country we were lucky – only 1 case was diagnosed in the UK and this was identified relatively promptly with no secondary infections. Was the money and time spent on preparedness wasted? Clearly not, as a different throw of the dice could have had catastrophic consequences without it and the work will serve us well should another similar threat emerge in the near future. Investment in infection prevention and control, therefore, must be resolutely defended when there are so many competing priorities.
David Partridge
Consultant Microbiologist and Infection Control Doctor
Honorary Senior Clinical Lecturer
Florey Institute for Host-Pathogen Interaction, University of Sheffield
Communications Secretary
British Infection Association
Tel: +44 (0)1565 632 982
Editor's Recommended Articles
-
Must Read >> Fighting back against antibiotic resistance