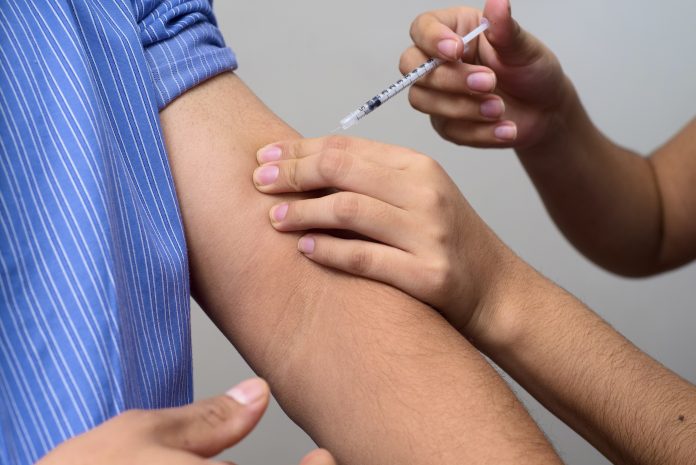
Cyndi Williams, Co-Founder and CEO of Quin, explores the stress of making diabetes decisions when it comes to injecting insulin
People with no experience of diabetes often have misconceptions about injecting insulin. They assume it’s a straightforward treatment: the doctor recommends a dose, the patient injects it, and all is well. The reality is far more complex, and there are as many different regimes for treating diabetes as there are people with diabetes.
There is no single dose of insulin that suits everybody, every day. The amount a person with diabetes needs to inject varies based on dozens of complex factors, including diet, exercise and menstruation, as well as seemingly minor lifestyle choices like taking a hot shower. Further, if a person injects too much or too little insulin, there could be significant health consequences.
Medical recommendations for diabetes offer only generic formulas for calculating doses and many people with diabetes report that these guidelines are unhelpful. In a recent survey of people with diabetes, 46% reported regularly needing to adjust their insulin doses because the medical guidance didn’t match their lived reality.
Decisions, decisions
People with diabetes make an incredible number of critical health decisions every day, and that can have a significant impact on their mental health.
In 2014, Stanford University researchers estimated that people living with type 1 diabetes make an additional 180 additional health-related decisions every day compared to people without diabetes – that’s equivalent to around one decision every five waking minutes.
People with diabetes need to make decisions about how much insulin to inject, as well as other related decisions like what and when it is safe to eat, when to inject, when to measure their blood sugar, and what activities they can safely participate in. Fundamentally, people with diabetes are running a constant mental equation and weighing dozens of factors to make decisions that affect their immediate health.
Having diabetes includes all the decision-making of a high-stress job – and making the wrong decisions could land a person in hospital.
Despite the prevalence of this experience among people with diabetes, the medical establishment has not conducted enough serious research into it or invested enough in supporting people through it.
Mental health consequences
Taking on these decisions every day takes a toll on people’s mental health. Research found that 55% of respondents with type 1 diabetes experienced anxiety and stress, 46% experienced depression, and 50% experienced increased fatigue. In some cases, this can culminate in a phenomenon called “diabetes burnout,” a sense of exhaustion and frustration which is often associated with depression and anxiety. Some research has even suggested that it is the condition itself that causes depression, rather than the experience of managing it.
To overcome these issues, people with diabetes need greater support. Two-thirds of the respondents to Quin’s survey reported seeing a GP – the primary point of care for people with diabetes – three times each year or less. This leaves them almost entirely unsupported when it comes to making the everyday decisions that affect their health and wellbeing.
Even in an ideal situation, no doctor could assist a person with 180 decisions every day. Instead, we must look to technology to better support people with diabetes. Technologies, such as continuous glucose monitors and apps, empower people to better understand and manage their blood sugar when they’re on their own. This is better for their mental and physical health. We can’t yet make the personal trial-and-error go away, but we can honour the people who do it and give them the tools to do it better and have a significantly higher quality of life.