Steve Jones, President of EU-IPFF and Chair, Action for Pulmonary Fibrosis in the UK describes the connection between COVID-19 and pulmonary fibrosis
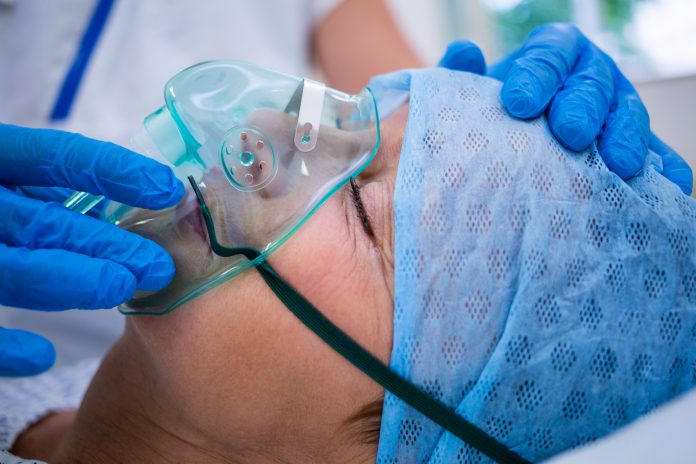
Imagine every breath you take is an effort. That is what it is like for many people recovering from COVID-19 and for over 250,000 people in Europe1 living with the devastating lung disease, pulmonary fibrosis.
Pulmonary fibrosis is the fifth biggest respiratory killer in Europe after lung cancer, COPD, pneumonia and COVID-19. It accounts for over 1% of all deaths and kills more people than either leukaemia or ovarian cancer. Despite this, very few people are aware of the disease.
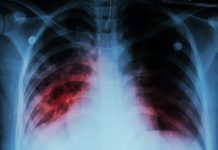
Pulmonary fibrosis causes scarring or stiffening of the lungs, making it hard for oxygen to pass from the lungs into the body. Early symptoms of the disease include a persistent cough and breathlessness. Over time, people find it increasingly difficult to breathe even becoming breathless when eating or talking. Everyday tasks many take for granted become increasingly hard. In time, patients become dependent on oxygen and ultimately die from respiratory failure.
Every 15 mins, somebody in Europe dies of pulmonary fibrosis.
As we live through the COVID-19 epidemic, pulmonary fibrosis patients understand, perhaps better than most, what COVID-19 feels like. When people recovering from COVID-19 say that walking across the room feels like climbing Mount Everest, pulmonary fibrosis patients understand.
Pulmonary fibrosis describes a group of conditions, many of which are ’progressive’ in the sense that they get worse over time, often quite rapidly2. People affected by these diseases have a low life expectancy of just three to five years from diagnosis – a worse prognosis than most major cancers.
Idiopathic pulmonary fibrosis (IPF)
The most aggressive form of the disease is idiopathic pulmonary fibrosis (IPF). Although the cause of IPF is not known, scientists believe it is triggered, in people with a pre-existing genetic susceptibility, by exposure to cigarette smoke, dust and pollution.
Acid reflux may also play a role. Epidemiological research indicates that the incidence of IPF is increasingly rapidly at 2-3% annually3.
In the last few years, two antifibrotic drugs have become available, which slow the progress of IPF and may extend life by about two years. The European Medicines Agency (EMA) has recently approved one of these drugs for use across all types of progressive pulmonary fibrosis, potentially more than doubling the number of patients in Europe receiving antifibrotic medication.
Despite the grave prognosis for people affected by pulmonary fibrosis, there is hope. New anti-scarring drugs are in the pipeline and other treatments are being developed for the debilitating IPF cough, which affects 70% of patients. Moreover, new genetic insights into the disease raise the prospect of precision medicine using targeted interventions tailored to patients with specific genetic or molecular abnormalities.
Although pulmonary fibrosis is a deadly disease and is killing more and more people each year, increased collaboration among doctors, scientists and patient advocacy groups is leading to real improvements in outcomes for patients. The European Idiopathic Pulmonary Fibrosis and Related Disorders Federation (EU-IPFF), plays a role in providing a forum for discussion and voicing the concerns of patients directly and through its 21 member organisations across Europe.

COVID-19 and pulmonary fibrosis
COVID-19 differs from pulmonary fibrosis in being an infectious disease caused by a newly discovered coronavirus. Most people with COVID-19 experience mild to moderate respiratory disease and recover without requiring special treatment. Older people (over 60 years of age) and those with underlying medical conditions, such as heart disease, hypertension, diabetes or obesity, are more likely to develop serious illness and require hospitalisation. Some of these patients may go on to develop pulmonary fibrosis. Interestingly, this is the same broad group of people who most commonly get IPF.
By late August 2020, 2 million COVID-19 cases had been registered in Europe and 180,000 people had died from the disease. Three-quarters of those affected recovered without needing special treatment, while approximately 500,000 people had been hospitalised. About 15% (75,000 people), required intensive care and/or respiratory support, though there is considerable variation among countries.
Although doctors expect COVID-19 to result in continuing respiratory problems for many patients, we do not yet know how many will go on to develop progressive pulmonary fibrosis. But, given the large number of people hospitalised, there is likely to be a significant increase in the number of people living with pulmonary fibrosis in Europe.
Both COVID-19 and pulmonary fibrosis cause severe injuries to the lungs. In the case of COVID-19, the rapid onset of widespread inflammation can lead to injury and require mechanical ventilation, which may also damage the lungs. Conversely, in the case of pulmonary fibrosis, the injury is often insidious and results from prolonged exposure to inhaled matter. The original cause of the injury is often not known until it is too late, if at all. Asbestosis, for example, may result in rampant fibrosis decades after exposure to asbestos fibres.4
Improving outcomes for all people
Acute lung injury by itself is not sufficient to cause progressive lung scarring – the body’s repair systems must also fail. Scientists are beginning to understand the genetic and molecular level factors involved in progressive lung scarring in pulmonary fibrosis. They are reasonably confident that similar processes are at work with COVID-19, but more research is needed. As Professor Gisli Jenkins of the University of Nottingham, UK, puts it: “If we are to deal with the emerging epidemic of fibrotic lung disease and the very immediate COVID19 pandemic, it is vital we understand the similarities between these two conditions in terms of cell injury and failures in lung repair. This will ultimately help us to improve outcomes for all people with scarring conditions of the lung.”5
References
1 EU/EEA/UK.
2 These include idiopathic pulmonary fibrosis (IPF), chronic hypersensitivity pneumonitis (conditions like farmers’ lung and bird keepers’ disease) and auto-immune conditions where lung fibrosis is associated with disease such as rheumatoid arthritis.
3 Hutchison, J et al. 2014. Increasing global mortality from idiopathic pulmonary fibrosis in the twenty-first century. Annals ATS, Volume 11, Number 8, pp 1176-1185.
4 Gisli Jenkins, 2020. Demystifying Pulmonary Fibrosis. American Journal of Physiology, Lung Cellular and Molecular Physiology, August.
5 Personal communication. 25th August 2020.