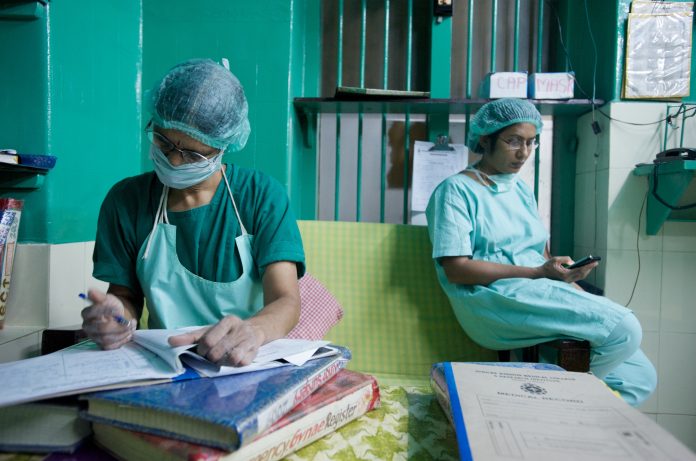
India broke records on Thursday (23 April) as more than 310,000 new COVID cases were documented – is the Indian ‘double mutation’, B1617, as infectious as the UK mutation?
Right now, the eyes of the world are on India. With a country-high of 310,000 new infections logged in one day, observers are trying to understand if there is a new, highly infectious mutation in circulation.
India has atleast 15,930,900 confirmed cases and 184,657 people are now dead.
Currently, healthcare professionals in India are denying that there is a link between the ‘double mutation’, B1617 and drastic rises in deaths, but they are continuing to invesigate. In India, 771 variants of concern have been detected so far. This includes 736 samples of the UK mutation, with a further 34 of the South African mutation detected.
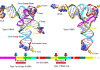
What is the B1617 mutation?
Scientists are calling it a ‘double mutation’, because there are two changes to the crucial spike protein – which can theoretically help the virus to escape being identified by the immune system, especially when the immune system has not been vaccinated.
Currently, there is not enough evidence that analyses this new form of COVID. Sequencing in India has found 412 of 9,115 variants sampled to be the new ‘double mutation’. This does not mean that the variant is not common – it just means that enough samples have not been genetically tested to track the mutation accurately.
The B1617 variant has been found in 21 other countries, including the UK.
When it comes to responsibility for the stark increase in deaths and hospitalisations, several other elements come into play – such as social distancing measures and vaccination rates.
Over 17 million people have been fully vaccinated, with a further 109 million on their first dose. But with a population of 1.36 billion, herd immunity is a long way off – especially since the rise in cases has slowed vaccination efforts. A previously outlined goal of 250 million fully vaccinated by July, 2021, is receding into the distance.
Lessons from the UK mutation?
The UK mutation, B117, originated in Kent. It is known to be atleast 45% more infectious than the original form of the virus, but not more deadly. This mutation was partially blamed for the winter wave of deaths in the UK, which saw increased hospitalisations and infection rates. It is extremely common for viruses to mutate multiple times, but the real issue is if vaccines can keep up – especially with mutations that are left relatively untreated for long periods of time.
In some poorer countries, vaccination not expected until 2023. These countries are locked out of vaccination due to drug prices or intellectual property laws, which stop them from making any. The delay in creating antibodies plus the need for local economies to open, creates a perfect breeding ground for COVID mutations.
All vaccines tested against B117 have taken an hit in efficacy. They are still functional, with studies on Pfizer showing the vaccine can still prevent 100% of hospitalisations and deaths against the South African mutation.
Essentially, the speed of transmission is increased because there is a higher likelihood of infection. The level of infection has decreased from February to March by 60%, according to the ongoing REACT study.
Vaccinate 50% of the older population to survive
Dr Dan Yamin, from the Laboratory for Epidemic Modeling and Analysis (LEMA) at Tel Aviv University, said: “Our message to the world is that if with our problematic starting point a distinct decline was identified, other Western countries can certainly expect the curve to break – despite the high contagion of the British variant – with a dramatic drop in severe cases following the vaccination of 50% of the older population, alongside targeted testing at risk epicenters.”
Vaccination appears to be working to stop COVID, even when they run up against mutations of concern like B117.