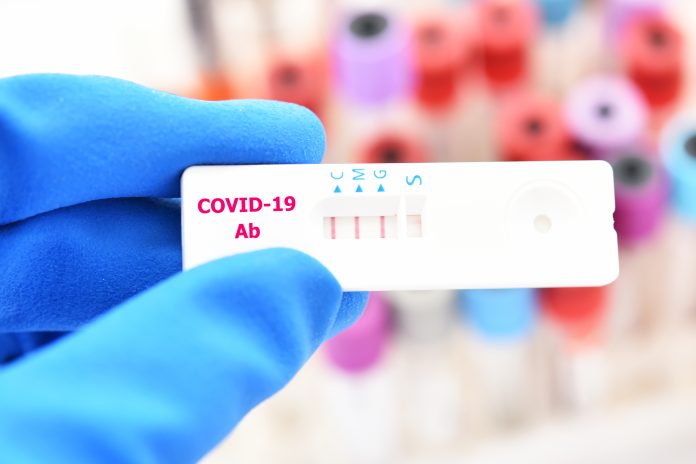
According to a new study, a third of leukaemia patients fail to generate an antibody response following two COVID-19 vaccine doses
Researchers from the University of Birmingham recruited 500 patients with chronic lymphocytic leukaemia to investigate their COVID-19 antibody response following vaccination.
41% had received two doses of the Pfizer BioNTech vaccine and 59% had received two doses of the Oxford AstraZeneca vaccine.
Blood samples were taken between 2-3 weeks following their second vaccination and again up to 30 weeks later. The results were compared to 93 age-matched healthy ‘controls’.
The results found that antibody responses were seen in only 67% of the leukaemia patients compared to 100% of age-matched controls.
In the 27% with leukaemia who did generate an antibody response, the average antibody level was 3.7 times lower than the healthy controls.
The researchers also found that those with leukaemia most likely to fail to respond to COVID-19 vaccination are:
- Men (with a 46% reduction)
- Patients being treated with Bruton tyrosine kinase inhibitor (BTKi) therapy (80% reduction)
- Those with a history of infection who require regular antibiotics (72% reduction)
- Those with low serum levels of two types of immunoglobulin known as IgA and IgM (72% and 57% reduction respectively).
Wuhan and Delta
Using serum samples from 94 leukaemia patients and 94 healthy controls, the team also analysed their ability to neutralise live infection using the Wuhan virus and the Delta variant.
In the healthy cohort, 96% neutralised the Wuhan virus and 84% the Delta variant. However only 62% of leukaemia patients neutralised the Wuhan virus and 14% the Delta variant.
Dr Helen Parry, a National Institute for Health Research (NIHR) academic clinical lecturer at the University of Birmingham, said:
“It is concerning that 33% of patients in our study did not generate any measurable antibody response to two doses of COVID-19 vaccination, and particularly concerning that in those who did generate an antibody response, there was a profound loss in ability to neutralise live Delta variant.
“The Delta variant is now globally dominant and more than twice as contagious as the Wuhan virus.
“Current COVID-19 vaccines are based on the spike protein sequence from the original Wuhan virus, whereas the Delta variant contains additional mutations.”
The scientists also analysed how antibody responses differed depending on the stage and treatment of the disease:
- Those who have never been treated but are under active monitoring had the highest antibody response rates (79% positive response)
- Antibody response rate was lowest in patients who were actively being treated (43%).
- 56% antibody response seen in patients who had completed anti-CD20 therapy more than 12 months prior to their second vaccine – compared to 24% in those whose CD20 therapy ended less than 12 months prior to double vaccination.
Dr Graham McIlroy, clinical research fellow at the University of Birmingham, says:
“This finding suggests that vaccination should be encouraged in patients who are in remission at least one year after anti-CD20 therapy.”
Further investigation found that antibody titers in leukaemia patients who had previously been infected with COVID-19 were 21-times higher than those in patients without infection.
The leukaemia patients without previous COVID-19 infection had equal antibody responses no matter which of the two vaccines they had received.
Dr Graham McIlroy added: “This provides evidence that both mRNA and adenovirus-based vaccines provide equal efficacy in leukaemia patients, and it is important we assess this further by analysing the antibody response to other COVID-19 vaccines currently being used around the world.”
Paul Moss, Professor of Haematology at the University of Birmingham and principal investigator of the UK Coronavirus Immunology Consortium (UK-CIC), concluded:
“The rapid development of vaccines for COVID-19 has been a major step forward in the battle against this global pandemic, however, our findings argue strongly that further protection for this vulnerable cohort is needed.
“A third vaccine dose is likely to boost antibody responses in some patients, but there are additional complications in leukaemia patients and additional medical interventions may be required.
“What is encouraging is that we found that in those who did generate an antibody response this increased 294-fold between their first and second vaccines, which may bode well for the use of an additional third booster vaccine.
“We will now continue to assess antibody responses prospectively and following third booster vaccination.
“We would continue to encourage all people, and especially those patients within these clinically at-risk groups, to make sure they receive their vaccine doses if they haven’t done so already.”
Dr Jonathan Pearce, Director of the COVID-19 Response at the Medical Research Council (MRC), which is part of UKRI and co-funded the study, said:
“This study increases our understanding of how people with leukaemia respond to the COVID-19 vaccine, helping us to identify key at-risk patient groups who don’t develop a strong immune response.
“For at-risk people, it highlights the importance of additional protection measures, including third doses.
“Currently the MRC and Vaccines Taskforce funded OCTAVE DUO study is investigating third vaccine doses in people with weakened immune systems.”
The research was funded by the National Core Studies Immunity programme which is funded by UK Research and Innovation (UKRI) and was also partially supported by UK-CIC which is jointly funded by UKRI and NIHR.